You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Disclosures: The author had no disclosures to report.
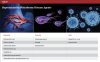
Infections and diseases caused by waterborne organisms remain a major source of global morbidity and mortality.1 These include pathologies caused by a variety of bacteria, protozoa, viruses, and intestinal parasites. Many are able to thrive and proliferate in contaminated natural water sources as well as in man-made systems containing waterlines designed to provide water for public consumption, building equipment, and use in healthcare facilities. While certain well-known bacterial pathogens (ie, Salmonella Typhi, Vibrio cholerae, Escherichia coli) are responsible for a substantial portion of the disease burden, especially in developing countries, a number of new pathogens transmitted by contaminated water have been described in recent decades. These include Cryptosporidium parvum (1976), Legionella pneumophila (1977), and noroviruses (1972), as well as more virulent strains of previously known bacteria, such as Vibrio cholerae O139:H7 (1992). A partial list of major infectious agents that can be spread by water is presented in Table 1.
In 1854, the first documented outbreak of waterborne disease was traced to a contaminated public well in London, England. This initial epidemiological study by Dr. John Snow determined that the consumption of water from a sewage-contaminated well led to cholera in people who drew water from that source.2 The publication of Snow’s groundbreaking Broad Street Pump investigation was the first step in establishing a new scientific discipline aimed at studying organisms capable of spreading disease through water contamination. Although it is a much bigger problem in developing countries, waterborne diseases also pose a threat in the United States and other countries with established water treatment procedures and infrastructures.
Government-mandated sanitation laws began to appear in the later part of the nineteenth century. These laws were designed to facilitate better handling and disposal of sewage and the use of filtration and chlorine treatment for the disinfection of drinking water. Although these routine procedures dramatically improved water supply safety, we continue to see emerging and persistent public health challenges related to infection from drinking water, recreational water, and water used in healthcare facilities. For example, the US Centers for Disease Control and Prevention (CDC) reported 32 documented drinking water outbreaks in the United States from 2011 to 2012, which resulted in at least 431 cases of illness, 102 hospitalizations, and 14 deaths. Strains of L. pneumophila were responsible for two thirds of these outbreaks.3
In some instances, hundreds and even thousands of people can be infected during a single outbreak. For example, in 1976, Philadelphia experienced a Legionnaires’ disease epidemic, in which attendees at an American Legion convention developed a previously unspecified clinical infection from an undetermined water source at their hotel. In total, 221 people were affected and 31 people died from what was later determined to be respiratory infection caused by L. pneumophila.4 In 1993, the water system for the city of Milwaukee was contaminated with Cryptosporidium, a chlorine-resistant, highly pathogenic protozoan parasite known to be responsible for many illnesses and deaths throughout the world.5 This organism infected approximately 400,000 people, making the incident the most serious waterborne disease outbreak in US history.5 These and other microbes have also been found to be responsible for clinical infections involving hot tubs, swimming pools, air conditioners, and cooling towers.
Waterborne Infections in the Healthcare Environment
There is extensive clinical and microbiological evidence documenting waterborne infections originating in hospital settings. Follow-up investigations looking for the causes of illness indicated that a variety of organisms can survive and reproduce in contaminated water sources, thereby presenting a potential source for subsequent transmission to susceptible patients. Localized skin infections, bacteremias, and more severe disseminated diseases can develop, especially when infection occurs in immunocompromised hosts and/or critically ill patients. Table 2 lists the types of hospital water reservoirs involved in these outbreaks.6 With specific regard to dentistry, demonstration of microbial contamination in dental unit water systems was first reported in high-speed handpiece lines by Dr. G.C. Blake in 1963.7 Subsequent research has further delineated, characterized, and described microbial interactions and their biofilms in waterlines.8,9 Most isolated organisms are aquatic, gram-negative bacteria that typically enter the dental unit from the municipal water supply. Many are able to thrive in this low nutrient, low temperature environment and are major components of resultant biofilms that form on the walls of waterline tubing. Oral flora can also be found in dental unit water; however, they are less adapted to flourish in that environment. They enter waterlines during patient treatment through the retraction of oral fluids into handpieces or air/water syringes and can remain for extended periods. Effective anti-retraction valves are able to reduce the potential for these organisms to enter equipment. Among the microbial classes recovered from colonized water samples, Pseudomonas, Legionella, and species of nontuberculous mycobacteria (NTM), such as Mycobacterium abscessus, are among the most notable. It is also of interest to note that L. pneumophila and M. abscessus have been identified as the bacterial agents associated with reported infection outbreaks in dental patients.10-12
As investigations continue into these recent L. pneumophila and M. abscessus dental water transmissions, it is useful to briefly review the important characteristics of these bacteria regarding their ability to thrive in water and their potential to cause infections in both immunocompetent and immunocompromised individuals. It is not within the scope of this review to detail the clinical conditions; however, excellent resources are available, including the representative publications listed in the references.13-17
Legionella
Legionella species are gram-negative, rod-shaped bacteria that are routinely found in a wide range of aqueous environments and can proliferate at temperatures above 25°C. They have fastidious growth requirements, which could partially explain why Legionella infections were not recognized and diagnosed until the late 1970s. They are generally found in low concentrations as natural flora in many freshwater environments (eg, rivers, streams, lakes). They also thrive in a number of man-made water environments, such as cooling towers, evaporative condensers, air conditioning systems, hot tubs, and spas, which provide the bacteria with the appropriate temperatures for growth. Warm water (25°C to 50°C) provides support for high concentrations of these bacteria. Although Legionella are sensitive to disinfection, they are intracellular parasites, which provides an excellent survival advantage in both the water they colonize and during human infection. The ability of Legionella to infect and multiply in free-living amoebae provides added safety for the bacteria by allowing them to survive environmental pH changes, the absence of nutrients, or temperature alteration until more favorable aqueous conditions permit them to be released.
Infection with Legionella begins with the inhalation of aerosols containing bacteria into the lungs. Research indicates that these aerosols have been generated by contaminated water from cooling towers, warm water plumbing systems, humidifiers, spas, recirculating water systems, and now contaminated dental waterlines can be added to the list of sources.10 Evidence from some documented cases suggests that microaspiration may also serve as a route of infection. For this route, a specific infectious form of Legionella is not known; however, several naturally occurring states offer possibilities. These include biofilm particles and other microbes containing Legionella and free-flowing, extracellular planktonic Legionella. It is also possible that bacteria contained within protozoan cysts can serve as another type of infectious agent. There is no documented evidence of person-to-person transmission.13
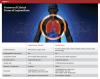
Although Legionella species are ubiquitous in many aqueous environments, they rarely cause disease. Despite this fact, L. pneumophila is the most commonly reported cause of waterborne legionellosis infections and outbreaks among humans. These organisms are not typically considered to be highly virulent pathogens; instead, they are classified as “opportunistic pathogens” and frequently found to cause respiratory disease manifestations in immunocompromised individuals. Infection develops after aerosolized bacteria enter the lungs, where they are encountered by alveolar macrophages and phagocytized. Next, the bacteria produce virulence factors that allow the engulfed Legionella to both survive and replicate within the inflammatory cell. Eventually, the macrophage lyses, and the increased concentration of bacteria is released to affect other phagocytic cells. As the microbial concentrations increase dramatically, other cells (eg, neutrophils, other macrophages, erythrocytes) infiltrate the alveoli, resulting in increased capillary permeability (ie, edema). Two clinical forms of legionellosis are known: Legionnaires’ disease and Pontiac fever (Table 3).13,14
M. abscessus
Mycobacteria are divided into two major groups: the Mycobacterium tuberculosis complex, of which M. tuberculosis is the only member, and the NTM, which includes all other mycobacterial species that do not cause tuberculosis or leprosy. Along with a number of other species within this latter group, M. abscessus is an environmental organism that is commonly found in soil, water, and dust. In contrast to the slower-growing M. tuberculosis, NTM produce visible cultures in vitro within 7 days.
Their recognized role in clinical infections has increased in recent years, in part because of laboratory advances in species identification, which have been better able to differentiate the various NTM. As a result, investigations of clinical diseases have now shown that M. abscessus can cause a variety of chronic infections, affecting skin, soft tissues, lungs, and ocular tissues. Many of the diagnosed infections have been associated with surgical and other procedures affecting the integrity of the skin, such as cosmetic surgeries, tattooing, or acupuncture.15,16 M. abscessus is also very resistant to the standard antibiotics used to treat tuberculosis and most other antimicrobial agents. As expected, drug susceptibility testing is important in achieving effective chemotherapy against infection.
It should be emphasized that tap water is considered to be a major reservoir for M. abscessus and other NTM, and that this vehicle has been traced as a source for patient exposure and resultant clinical infection. This fact is especially pertinent when considering the recent outbreaks involving this organism in pediatric dentistry offices. Evidence suggests that a number of patients were infected from treatment water used during pulpotomy procedures.11,12 Another challenge for healthcare settings is that NTM have also been isolated from contaminated medications and medical devices.17 Modes of documented bacterial transmission include direct contact with contaminated water or material following traumatic injury and environmental exposure. The infection caused by M. abscessus is somewhat different from the illnesses caused by other rapidly growing NTM, in that it can cause disease in both normal, immunocompetent hosts as well as in individuals who are immunosuppressed. In addition, it is considered an emerging pathogen among cystic fibrosis patients and those undergoing lung transplantation. This characteristic expands the primarily opportunistic pathogenic role of these bacteria, in that it can also cause disease in healthy individuals who are exposed. This fact was borne out during the investigation of recent infections in two pediatric dentistry practices, as the infections caused by M. abscessus occurred predominately in healthy young children.11,12
Conclusion
One does not have to look very far to find reminders of the importance of safe water. Infectious disease epidemics from contaminated drinking water have killed millions over the centuries, and they remain an ongoing threat to the wellbeing of people in many countries. As discussed above, many different types of micro- and macro-organisms thrive in aqueous environments and can cause devastating illnesses in infected individuals. However, progress has been made in a number of areas, especially with the construction of more effective pipeline infrastructures and treatment facilities, implementation of routine filtration and disinfection procedures, and monitoring of water supplies for possible contamination. In brief, good health is dependent on a clean, potable water supply.
Epidemiologic investigations of diseases occurring in the public water supply and in healthcare settings now use improved tracking and detection procedures that were not available a few decades ago. Current laboratory culture and microbial characterization techniques are also better able to isolate relatively new pathogens, such as the Legionella and Mycobacterium species discussed here. In addition, a better understanding of the potential for microbial contamination in healthcare equipment waterlines has spurred the development of multiple infection prevention strategies to prevent water contamination. Appropriate implementation of these procedures and treatments is especially important as the number of immunocompromised patients receiving dental and medical care steadily increases. The safety of water used to provide care should remain a major consideration, not just for these individuals, but for everyone.
References
1. Pedley S, Pond K. Emerging issues in water and infectious disease. World Health Organization. 2003;1-22. Available at: http://www.who.int/water_sanitation_health/emerging/emerging.pdf. Accessed May 31, 2017.
2. Snow J. On the mode of communication of cholera. In: Clendening L, ed. The Sourcebook of Medical History. New York, NY: Paul B. Hoeber, Inc.; 1942:468-472.
3. Beer KD, Gargano JW, Roberts VA, et al. Surveillance for waterborne Disease outbreaks associated with drinking water - United States, 2011-2012. MMWR Morb Mortal Wkly Rep. 2015;64(31):842-848.
4. Fraser DW, Tsai TR, Orenstein W, et al. Legionnaires’ disease: description of an epidemic of pneumonia. N Engl J Med. 1977;297(22):1189-1197.
5. Mac Kenzie WR, Hoxie NJ, Proctor ME, et al. A massive outbreak in Milwaukee of cryptosporidium infection transmitted through the public water supply [published correction appears in N Engl J Med. 1994;331(15):1035]. N Engl J Med. 1994;331(3):161-167.
6. Kanamori H, Weber DJ, Rutala WA. Healthcare outbreaks associated with a water reservoir and infection prevention strategies. Clin Infect Dis. 2016;62(11): 1423-1435.
7. Blake GC. The incidence and control of bacterial infection in dental spray reservoirs. Brit Dent J. 1963; 115:413-416.
8. Mills SE. The dental waterline controversy: defusing the myths, defining the solutions. J Am Dent Assoc. 2000; 131(10):1427-1441.
9. Mills SE. Dental unit water and air challenges. In: Molinari JA, Harte JA, eds. Cottone’s Practical Infection Control in Dentistry. 3rd ed. Philadelphia, PA: Wolters Kluwer/Lippincott Williams and Wilkins; 2010:63-75.
10. Ricci ML, Fontana S, Pinci F, et al. Pneumonia associated with a dental unit waterline. Lancet. 2012;379 (9816):684.
11. Peralta G, Tobin-D’Angelo M, Parham A, et al. Notes from the Field: Mycobacterium abscessus infections among patients of a pediatric dentistry practice—Georgia, 2015. MMWR Morb Mortal Wkly Rep. 2016;65(13):355-356.
12. Kravarik J. Bacteria in dentist’s water sends 30 kids to hospital. CNN. Available at: cnn.com/2016/10/11/health/california-dental-water-bacteria. Accessed May 31, 2017.
13. Edelstein AH, Roy CR. Legionnaires’ disease and pontiac fever. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. Philadelphia, PA: Elsevier Saunders; 2014:2633-2644.
14. CDC. Legionella: about the disease. Available at: https://www.cdc.gov/legionella/about/index.html. Accessed May 31, 2017.
15. Lee MR, Sheng WH, Hung CC, et al. Mycobacterium abscessus complex infections in humans. Emerg Infect Dis. 2015;21(9):1638-1646.
16. Uslan DZ, Kowalski TJ, Wegenack NL, et al. Skin and soft tissue infections due to rapidly growing mycobacteria: comparison of clinical features, treatment, and susceptibility. Arch Dermatol. 2006;142(10): 1287-1292.
17. CDC. Mycobacterium abscessus in healthcare settings. Available at: https://www.cdc.gov/HAI/organisms/mycobacterium.html. Accessed May 31, 2017.
About the Author
John A. Molinari, PhD
Director of Infection Control
THE DENTAL ADVISOR
Ann Arbor, Michigan
Professor Emeritus
University of Detroit Mercy
School of Dentistry
Detroit, Michigan