You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Creating an optimal experience for patients is part of almost everything a dental practice does. It begins before ever meeting the patient and continues until well after each visit is over. The experience can vary from hours to days depending on the procedure. Ranging from how the new-patient phone call transpires, to the size and shape of the arms on the dental chairs, the practice should focus on caring for the people it serves.
Unfortunately, postoperative sequelae can cause patients to rate even the best dental experience negatively. It can prompt them to become concerned about the quality of the care provided and feel hesitant to return to the dental office for future treatment. It can also put them at greater risk of additional long-term jaw pain.
Postoperative jaw and muscle problems are common after dental procedures.1-4 Often the symptoms are not properly diagnosed and treated. What starts as an acute issue can lead to chronic headaches, jaw pain, or neck pain. Almost any dental procedure can potentially traumatize the jaw joint and muscles; however, the longer the procedure or the more downward force placed on the mandible, the greater the risk becomes. Not all patients have the same tolerance; some have a greater underlying risk of trauma to the temporomandibular joint (TMJ) and muscles. Being able to define and identify jaw joint and muscle strain/sprain (JAMSS), evaluate patients for preoperative risk factors, manage higher-risk patients and procedures, and effectively treat JAMSS are key skills practitioners should possess when providing patient care.
What is JAMSS?
JAMSS is the diagnostic term that describes an acute trauma to the joint or muscles. It is one of the most common sequelae to dental procedures, with research indicating that more than 50% of patients with temporomandibular disorders (TMDs) report that the initial onset of pain was a direct result of dental care.1-13 In one study of 164 patients with TMDs, trauma was the initiating factor in 50.6% of cases, with 61% of these cases coming from trauma and strain during dental treatment.1 Among young adult patients, it was found that 23% of all jaw pain cases had the onset after third-molar extractions.2,3
JAMSS typically presents with patients reporting one or all of the following symptoms: pain in front of their ear (acute jaw pain), inability to open (limited range of motion), pain, or inability to chew or speak (tenderness and dysfunction).1,6 The symptoms can last as little as a few days or as long as several weeks. For many patients whose symptoms are transient, they may never even seek follow-up care unless they are advised to watch for these symptoms. Other times, upon following up with the dental office they may be told that the symptoms are normal and perhaps to treat themselves with over-the-counter pain medication.
Unfortunately, when left untreated or treated improperly JAMSS can progress into chronic jaw pain, neck pain, or headaches.8,12-14 Identifying patients and procedures at higher risk of JAMSS, understanding the signs and symptoms, and quickly and effectively managing the condition can prevent patients from developing a chronic TMD or orofacial pain condition. Most people have experienced some form of “sprain” or “strain” in other parts of their bodies, and by using these semantics clinicians can help their patients draw upon their previous experiences to manage the situation; this approach can also help eliminate any potential social and emotional stigma.
Preventing and Managing JAMSS
It is important to prevent and, if necessary, treat (or manage) JAMSS. Preventing JAMSS is relatively simple; an easy-to-implement assessment5,7,9,10 categorizes patient risk factors and procedure risk factors into low, moderate, and high groupings (Table 1 and Table 2). Once the risk category has been determined, simple and effective management strategies can reduce incidence (Table 3). Additionally, risk assessment helps both the patient and dental team evaluate for any postoperative signs of JAMSS.
If signs or symptoms of JAMSS develop, timely management of the condition must be implemented. A protocol for rapid treatment efforts can help prevent the development of chronic pain.14 This process begins by asking patients to watch for any postoperative issues, having them come in to the office as soon as possible for an evaluation, and initiating therapy to manage JAMSS and resolve it. This process of risk assessment, evaluation, and management has been put into an easy-to-follow system called SAFE.11,15
What is SAFE?
SAFE stands for “Set-up for safety, Assessment, Follow, and Evaluate.” The system encompasses four steps designed to prevent and manage JAMSS in a dental practice. Recognizing the symptoms of JAMSS and treating the condition quickly and effectively are important, but prevention is crucial. Reducing the incidence of JAMSS begins with risk assessment of both the patient and the clinical procedure. The first three steps in SAFE have to do with prevention, and every member of the dental team is part of the process.
Set-up for Safety
The “S” (set-up for safety) in SAFE entails making sure the dental team has the information and tools necessary to prevent and manage JAMSS. Information is the foundation of behavior change. Every team member needs to understand what JAMSS is, how it happens, and the systems in place in the office for prevention and management. The team member who answers the phone, for example, needs to know what to listen for and what questions to ask the patient when taking the postoperative phone call. This will help him or her to take the appropriate next step in care. Often, patients’ symptoms are dismissed as normal. This can lead to a delay in management and a decrease in the effectiveness of simple treatment modalities aimed at a complete resolution. Ineffectual phone screening may also lead the patient to seek care outside of dentistry at, for example, an urgent care center or doctor’s office, where access to simple tools that effectively treat JAMSS may not be available.
Risk assessment may take place at a new-patient appointment, during a routine hygiene visit, or at the beginning of a procedure, and any member of the dental team can perform it. Bringing the whole team together and learning about JAMSS, walking through the questions on risk assessment (Table 1), and creating a system to implement assessment and management strategies are fundamental components of the first step of SAFE.
Set-up for safety also includes creating or obtaining written information on JAMSS to give to the patient. This can comprise educational material for patients on risk factors, warning signs, and symptoms, as well as postoperative instruction. Sharing this information in the form of written take-home postoperative instructions may be critical for some patients, as they can refer to it if they suspect they are having any symptoms. Additionally, patients at moderate to high risk or who are experiencing JAMSS may be given some postoperative exercises to perform (listed in Table 3), instructions on analgesics, and dietary precautions both verbally and in written form. The dental office can also disseminate information through use of digital signage in the waiting room, color trifold information sheets, or a blog on the office website. All of these methods are aimed at encouraging patients to share their suspicions if they believe they are at risk.
Set-up for safety also involves having the tools and materials available to prevent and manage JAMSS. A key element of patient risk assessment is the patient’s preoperative range of motion; therefore, the dental office operatories should be equipped with range-of-motion guides. The devices can be disposable plastic cards or sterilizable plastic or metal measurement devices; they can even be specialized mirror handles marked with measurements. For longer procedures that create more downward pressure on the jaw, a mandibular support that attaches to the dental chair may be useful. An interim dental splint (eg, QuickSplint®, Orofacial Therapeutics, LP, www.quicksplint.com) or a lucia jig relined with bite registration material can be fabricated and used preoperatively to minimize risk during a procedure. The device can be inserted periodically during a procedure to allow the patient to rest and take stress off the joint and muscles. It could be sent home with the patient for postoperative management. The aforementioned dental splint can also be used to treat JAMSS should it occur despite prevention efforts, or for an emergency patient who has JAMSS that is unconnected to a dental procedure.
In short, a list of materials, supplies, and patient information forms that the office needs to implement a JAMSS protocol should be made. Once everything has been acquired, it needs to be organized in the office and a system created for its use. Risk assessment forms and range-of-motion tools should be easily accessible in any operatory where an assessment may take place. Similar to how procedure bins are created in other areas of dentistry, a bin that contains all the materials and supplies for splint fabrication and JAMSS management can be assembled and moved into any operatory when needed.
Assessment
The JAMSS protocol employs a quick and easy-to-implement assessment—the “A” in SAFE—for determining preoperative risk, which can also function as a postoperative evaluation. The process starts with a 12-question verbal assessment with the patient, which generally takes just a few minutes (Table 1). Research suggests that the factors in this assessment are strong predictors of initial onset of TMD.5,7,9,10 The questions address pain on jaw opening, history of headache or facial pain, limited range of motion, emotional and general body factors, and potential stress.13-22
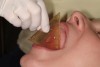
The next component of the risk assessment is obtaining a measurement of the patient’s pretreatment range of motion. The measurement can be obtained using a disposable or reusable measuring device (Figure 1), or the clinician can simply have the patient open comfortably and attempt to put three fingers between the upper and lower incisal edges. If the patient fails the “three-finger test” or has a comfortable opening that is either less than 40 mm or greater than 60 mm, he or she is no longer in a low-risk category.
The last area of assessment involves dental procedures. Some initiating factors for development of JAMSS are direct trauma due to a nerve block, sustained or forceful contraction of the muscles that can be worsened by use of a bite block, hyperextension of the muscles due to opening too wide, or prolonged stretching of the muscles.2-4,7-10 These factors have been merged and distilled down to a few simple questions about the procedure to assign a risk category. In general, the further back in the mouth the clinician will be working, the longer the procedure, and the more downward pressure being put on the mandible, the greater the procedural risk.
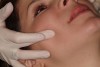
The combined results of the verbal assessment, range-of-motion test, and procedural assessment allow the clinician to determine a risk category of low, moderate, or high (Table 2). When a risk category of moderate to high has been determined, the JAMSS protocol can be used to minimize the incidence of risk by following suggested management strategies. In addition to management categories, patients who respond positively to questions on the verbal assessment and whose range of motion is outside of the 40 mm to 60 mm range would benefit from a more extensive evaluation of their jaw joints, muscles, and dentition (Figure 2). This examination should include identification of joint sounds, joint and muscle tenderness, and documentation of occlusal evidence of parafunction. Medical conditions like diabetes, arthritis, muscle disorders, and certain medications can also be contributing factors and should be reviewed with the patient.
Follow
The “F” in SAFE is for “follow” preventive strategies that will minimize the risk of JAMSS. For patients in a moderate to high risk category for developing JAMSS, the following suggested management strategies for prevention can be adhered to:
• Keep visits short, dividing complex care into segments when necessary.
• Schedule enough time to allow the patient rest periods (5 minutes each) during longer appointments or more stressful procedures.
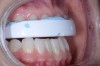
• Fabricate an interim dental splint (Figure 3) for the patient to use preoperatively when sleeping to help minimize existing inflammation and stress in the joints and muscles.
• Encourage patients to notify the clinician when they need a rest period.
• Avoid the use of bite blocks, as this increases sustained contraction of the muscles.
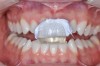
• Use an anterior deprogrammer (Figure 4) during rest periods on the day of the procedure.
• Use a dental splint postoperatively to aid in recovery of the joints and muscles.
• Prescribe anti-inflammatory medications for before and after the procedure.
• Apply heat packs to facial muscles during rest periods.
• Minimize downward pressure on the lower jaw or use a mandibular support device.
Evaluate
Finally, the “E” in SAFE is for “evaluate.” Patients should be evaluated for signs of JAMSS at the end of an appointment and postoperatively if they are moderate to high risk based on the clinician’s assessment. During a procedure, the clinician should watch for signs of strain, such as fluttering of the lower jaw, difficulty staying open, or patients trying to hold or rub their joint or muscles. The clinician should ask patients if they are having any discomfort or difficulty. These are indicators that a 5-minute break is in order, or that the dental splint should be worn or heat applied.
At the end of the appointment, the clinician should ask the questions on the JAMSS assessment (Table 1) and find out if the patient is currently experiencing any indicative factors, like jaw or muscle pain, headache, or difficulty opening. A postoperative range-of-motion measurement should be taken and compared to what was obtained before the procedure or at the examination appointment. For moderate- to high-risk patients, a postoperative evaluation appointment can be scheduled at which the clinician can again review the assessment questions with the patient and measure range of motion; this can be essential to early intervention. These patients should be given postoperative follow-up phone calls, and much of the assessment asked over the phone. Patients should be made aware of the signs and symptoms of JAMSS and be encouraged to call the office quickly if they notice any developing so they can be seen for an evaluation. Providing take-home patient instructions is critical, as many verbal instructions at the end of a long appointment may be missed.
If at any of the postoperative evaluation points pain or tenderness is discovered or reported, a decrease in range of motion is measured, or difficulty opening is reported, then a “speed-to-treat” protocol is initiated to treat JAMSS and maximize the chances of resolution.
Speed-to-Treat Protocol
To minimize the risk that the patient will develop chronic jaw pain, earaches, temple headaches, or jaw dysfunction, a “speed-to-treat” JAMSS protocol is recommended.17,20 The sooner the protocol is initiated, the better the outcome. Being alerted to these signs and symptoms on the day they develop is ideal. The protocol includes four steps, known by the acronym MEAT: movement, exercises, analgesia, and treatment (Table 3). This orthopedic model engages patients in their own self-care, guides them on monitoring their condition and instituting behavior change, and augments their recovery with a simple device that is both diagnostic and therapeutic. Completing these four steps maximizes the potential for success in reducing pain and dysfunction at the acute stage.
Movement. This includes self-care training on the proper use of the jaw and avoiding risk factors for delayed recovery. The protocol will guide patients to use their jaw, but to do so carefully in a way that allows for rest and recovery. This includes avoiding hard or chewy foods like bagels, tough meat, and nuts. Depending on the severity of the condition, some time on only very soft foods or liquids may be indicated. The patient should be encouraged to become aware of and limit risk factors such as clenching, grinding, nail biting, or other forms of overuse.
Exercises. Performing exercises that focus on stretching to restore natural range of motion can help patients return to normal function. In addition, posture and relaxation exercises will reduce strain to the muscles and encourage healing.23,24 These exercises are easy to do and can be given to the patient to take home in the form of written instructions. Online training programs are also available.25
Analgesia. Acetaminophen, anti-inflammatories, topical medication, or hydrotherapy (alternating heat and cold) can be used to achieve pain relief and help facilitate movement, exercise, and healing. Topical medication such as a 5% lidocaine patch or anti-inflammatory solutions overlying the muscle and joint may be particularly helpful in alleviating acute JAMSS for patients who are medically compromised or cannot tolerate systemic side effects of oral medications. Opioid medications, if used at all, should be short-term (<7 days) to prevent long-term opioid dependency if acute problems become chronic.
Treatment. A protective immediate oral appliance can be fabricated chairside to help protect the jaw and relax the muscles, similar to a protective elastic bandage for ankle or wrist injuries.26-29 Worn at night, the aforementioned dental splint can reduce jaw closing muscle activity (eg, jaw clenching or tooth grinding), inhibit the maximum bite force, and help encourage healing of acute temporomandibular pain and related restricted jaw opening.27-29 The flat occlusal surface of the splint allows the mandible to freely move in various directions instead of closing into a specific dental relationship, encouraging healing and normal function. A splint allows the clinician to place the patient on an appliance immediately, without the delay of lab processing and without the additional trauma of taking impressions and records needed for appliance fabrication. It is large enough to avoid aspiration risk, is comfortable, and also grants both the patient and the operator an opportunity to uncover parafunctional risk because the device will show evidence of wear. The splint is designed to be worn for a short time. Once acute symptoms are resolved a determination can be made regarding long-term parafunctional protection with an oral appliance.
Conclusion
Determining when patients are at functional risk, who would benefit from wearing an appliance, and when to complete a more extensive functional examination can be daunting. Both the JAMSS and SAFE protocols were developed to help patients avoid acute joint and muscle issues, but more importantly, to avoid the development of a chronic TMD or orofacial pain condition that these acute episodes can trigger. The protocols are easy to implement, and dental professionals can use them routinely as a screening tool. They can be used to identify patients at higher functional risk who would benefit from a more extensive evaluation, oral appliance therapy, and management strategies during dental procedures. In addition, they offer clinicians a quick, easy-to-implement treatment protocol for patients already experiencing symptoms. The initial steps are to make the entire team aware of JAMSS and SAFE, obtain the necessary materials, and integrate them into daily systems.
Questions
Queries to the authors regarding this CE may be submitted to authorqueries@aegiscomm.com.
References
1. Fricton JR, Kroening R, Haley D, Siegert R. Myofascial pain and dysfunction of the head and neck: a review of clinical characteristics of 164 patients. Oral Surg Oral Med Oral Pathol. 1985;60(6):615-623.
2. Contar CM, de Oliveira P, Kanegusuku K, et al. Complications in third molar removal: a retrospective study of 588 patients. Med Oral Patol Oral Cir Bucal. 2010;15(1):e74-e78.
3. Huang GJ, Rue TC. Third-molar extraction as a risk factor for temporomandibular disorder. J Am Dent Assoc. 2006;137(11):1547-1554.
4. Sahebi S, Moazami F, Afsa M, Nabavi Zade MR. Effect of lengthy root canal therapy sessions on temporomandibular joint and masticatory muscles. J Dent Res Dent Clin Dent Prospects. 2010;4(3):95-97.
5. Huang GJ, LeResche L, Critchlow CW, et al. Risk factors for diagnostic subgroups of painful temporomandibular disorders (TMD). J Dent Res. 2002;81(4):284-288.
6. Poveda-Roda R, Bagán JV, Jiménez-Soriano Y, Fons-Font A. Retrospective study of a series of 850 patients with temporomandibular dysfunction (TMD). Clinical and radiological findings. Med Oral Patol Oral Cir Bucal. 2009;14(12):e628-e634.
7. Stone J, Kaban LB. Trismus after injection of local anesthetic. Oral Surg Oral Med Oral Pathol. 1979;48(1):29-32.
8. Bakland LK, Christiansen EL, Strutz JM. Frequency of dental and traumatic events in the etiology of temporomandibular disorders. Endod Dent Traumatol. 1988;4(4):182-185.
9. Stacy GC, Hajjar G. Barbed needle and inexplicable paresthesias and trismus after dental regional anesthesia. Oral Surg Oral Med Oral Pathol. 1994;77(6):585-588.
10. Martin MD, Wilson KJ, Ross BK, Souter K. Intubation risk factors for temporomandibular joint/facial pain. Anesth Prog. 2007;54(3):109-114.
11.Fricton J, Eli B, Gupta A, Johnson N. Preventing chronic pain after acute jaw sprain or strain. JADA. 2016;147(12):979–986.
12. Pullinger AG, Seligman DA. Trauma history in diagnostic groups of temporomandibular disorders. Oral Surg Oral Med Oral Pathol. 1991;71(5):529-534.
13. Burgess J. Symptom characteristics in TMD patients reporting blunt trauma and/or whiplash injury. J Craniomandib Disord. 1991;5(4):251-257.
14. Häggman-Henrikson B, Rezvani M, List T. Prevalence of whiplash trauma in TMD patients: a systematic review. J Oral Rehabil. 2014;41(1):59-68.
15. Schiffman EL et al. The Research Diagnostic Criteria for Temporomandibular Disorders. V: methods used to establish and validate revised Axis I diagnostic algorithms. J Orofac Pain. 2010;24(1):63-78. 16. Humphrey SP, Lindroth JE, Carlson CR. Routine dental care in patients with temporomandibular disorders. J Orofac Pain. 2002;16(2):129-134.
17. Epker J, Gatchel RJ, Ellis E 3rd. A model for predicting chronic TMD: practical application in clinical settings. J Am Dent Assoc. 1999;130(10):1470-1475.
18. Zucuskie TG, et al. A controlled clinical trial of the usefulness of an external mandibular support device during routine dental care [master’s thesis]. Minneapolis, MN: University of Minnesota; 1996.
19. Fernandes P, Velly AM, Anderson GC. A randomized controlled clinical trial evaluating the effectiveness of an external mandibular support device during dental care for patients with temporomandibular disorders. Gen Dent. 2013;61(6):26-31.
20. Garofalo JP, Gatchel RJ, Wesley AL, Ellis E 3rd. Predicting chronicity in acute temporomandibular joint disorders using the research diagnostic criteria. J Am Dent Assoc. 1998;129(4):438-447.
21. Fillingim RB, Ohrbach R, Greenspan JD, et al. Psychological factors associated with development of TMD: the OPPERA prospective cohort study. J Pain. 2013;14(12 suppl):T75-T90.
22. Slade GD, Fillingim RB, Sanders AE, et al. Summary of findings from the OPPERA prospective cohort study of incidence of first-onset temporomandibular disorder: implications and future directions. J Pain. 2013;14(12 suppl):T116-T124.
23. Dall Arancio D, Fricton J. Randomized controlled study of exercises for masticatory myofascial pain. J Orofac Pain. 1993;7(1):117.
24. Fricton J, Velly A, Ouyang W, Look JO. Does exercise therapy improve headache? a systematic review with meta-analysis. Curr Pain Headache Rep. 2009;13 (6):413-419.
25. Toolkits resources page. Preventing Chronic Pain website. https://www.preventingchronicpain.org/drupal/pcpnet/toolkits. Accessed February 20, 2017.
26. Wright EF, Domenech MA, Fischer JR Jr. Usefulness of posture training for patients with temporomandibular disorders. J Am Dent Assoc. 2000;131(2):202-210.
27. Maloney GE, Mehta N, Forgione AG, et al. Effect of a passive jaw motion device on pain and range of motion in TMD patients not responding to flat plane intraoral appliances. Cranio. 2002;20(1): 55-66.
28. Komiyama O, Kawara M, Arai M, et al. Posture correction as part of behavioural therapy in treatment of myofascial pain with limited opening. J Oral Rehabil. 1999;26(5):428-435.
29. Magnusson T, Syrén M. Therapeutic jaw exercises and interocclusal appliance therapy. A comparison between two common treatments of temporomandibular disorders. Swed Dent J. 1999;23(1):27-37.
About the Authors
Lee Ann Brady, DMD
Founder
www.leeannbrady.com
Private Practice
Glendale, Arizona
James Fricton, DDS, MS
Professor Emeritus
University of Minnesota Schools of Dentistry
Medicine, and Public Health
Minneapolis, Minnesota
Private Practice
St. Paul, Minnesota
Brad Eli, DMD, MS
Private Practice Specializing in the Diagnosis and Treatment of Orofacial Pain and Sleep Disordered Breathing
Encinitas, California