You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
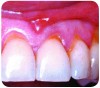
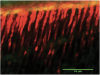
Dentin hypersensitivity has been cited as one of the most frequent complaints of those seeking dental treatment.1 Many people have encountered tooth sensitivity at some stage throughout their lives, and surveys have shown the condition to be very common2-4 particularly among those associated with gingival recession (Figure 1) or excessive enamel wear (Figure 2). Whereas there may be many individual causes of the symptom described as tooth sensitivity (Table 1), the diagnosis of the condition of dentin hypersensitivity can be a challenge, and appropriate differential diagnosis is essential to identify the cause.
Many patients do not realize that the tooth sensitivity they frequently encounter is not normal and can be relieved by their dental professional. For many sufferers dentin hypersensitivity has a very gradual and insidious onset and the fault is seen more with stimulus: the ice in the drink, the very cold water or cold air in Northern climates in winter, or the hot coffee, rather than with the exposed dentin of their teeth. These sufferers—often without realizing it themselves—develop a variety of coping strategies such as using less ice in cold drinks, allowing hot drinks to cool, brushing teeth with warm water, or drinking with a straw to direct cold drinks away from sensitive teeth. Oral hygiene may be compromised by avoidance of contact with the toothbrush bristles in sensitive areas. Many sufferers do not complain during regular check-ups and a problem is only noticed by an airblast during the examination or use of a scaling instrument during a cleaning. Only when interviewed further by the clinician do patients realize how much their case of sensitivity has led to the coping behaviors they gradually adopted and how much the condition has been allowed to interfere unnecessarily with their daily life.
Definition and the Need for Differential Diagnosis
The most widely accepted definition of this condition, formed by an expert panel of researchers and first published in 1997,5 states that dentin hypersensitivity is characterized by a short, sharp pain arising from exposed dentin in response to stimuli—typically thermal (hot and cold), evaporative (air blast or inhalation), tactile (touch or pressure), osmotic (sugar, syrup), or chemical (acids)—which cannot be ascribed to any other defects or pathology.
Further consideration of this definition indicates the following four specific elements, being:
• the nature of the pain;
• the occurrence in areas of exposed dentin;
• an identified stimulus; and
• the exclusion of any other possible diagnosis.
It is imperative to rule out active pathologic conditions (eg, tooth fracture, pulp inflammation, etc.) prior to providing any treatment of tooth sensitivity. Other conditions may also share similar symptoms and therefore a differential diagnosis is essential. Common confusing conditions may include fractured cusps and restorations, failing or leaking restorations, reversible pulpitis, and developmental defects where the coronal dentin is not covered by enamel (such as palatal–gingival grooves on lateral incisors), as well as a recent history of tooth whitening, placement of restorations, or periodontal procedures. In addition to the necessary differential diagnosis, a follow-up assessment after treatment is needed to ensure the symptoms have subsided, which, if so, will help confirm the initial diagnosis. In the event the patient is fully compliant with the recommended treatment and any modifications to diet or oral hygiene practices that may have been advised, but the presenting symptoms have not subsided, it is necessary to review the original diagnosis. As the diagnosis of dentin hypersensitivity is arrived at only by the exclusion of conditions that share similar symptoms, the follow-up review of the patient’s condition is essential. If the first line of treatment has not been totally successful, another possible diagnosis should be considered and the treatment plan modified accordingly.6 It is important to recognize that two or more etiologies may co-exist. If the original single diagnosis of dentin hypersensitivity is confirmed, then it may be appropriate to change the treatment plan.
Mechanisms
• To be hypersensitive, three conditions must be met in the dentin itself:
• dentin exposure to the oral cavity;
• open ends of dentin tubules of the exposed dentin; and
• entire path of open dentin tubules from the exposed dentin surface to the pulp.
Not all dentin tubules run the full width of the dentin, and not all tubules possess the mechanoreceptors that transmit the pain to the brain. As dentin exposure progresses, more tubules become exposed, and their diameter increases inversely to the distance from the pulp (Figure 3). The hydrodynamic theory for dentin hypersensitivity suggests that the stimuli trigger changes in the flow and pressure of the dentin tubule fluid that are detected by mechano-receptors around the odontoblasts and consequently perceived as the sensation of hypersensitivity. This theory helps explain the observation that for a tooth wear lesion the symptoms become more difficult to resolve by normal methods, largely due to more exposed tubules and wider tubules diameter.7
To gain a greater understanding of the structure of dentin and the perception of hypersensitivity, Absi studied caries-free teeth with exposed cervical root areas that were scheduled for extraction. Teeth were classified before extraction as being either non-sensitive or hypersensitive after suitable stimulation. After extraction the teeth were examined by scanning electron microscopy and the hypersensitive teeth showed approximately 8-fold more tubules per unit area than the non-sensitive teeth. Further, the tubule diameters were approximately doubled in the hypersensitive teeth compared to the non-sensitive teeth.8 The increased density of the tubules and the larger diameter will enable or allow a much greater flow of fluid in response to stimuli.
The varying number of dentin tubules and their size of diameter in hypersensitivity areas may help explain why some areas of exposed dentin are much more sensitive than others and also why not all exposed dentin is sensitive. It is important to recognize that personal perception of dentin hypersensitivity varies, and the tolerance level can also be different among individuals. Therefore, the severity of dentin hypersensitivity may not necessarily be proportional to the level of dentin exposure and/or strength of the stimuli for a particular patient.
Exposed dentin is often covered by a smear layer, which naturally occludes the tubule orifices (Figure 4). The smear layer is comprised of various salivary deposits such as glycoproteins and minerals as well as silica particles deposited from treatment agents, such as toothpaste. The intact smear layer is considered protective due to its occlusion properties. However it is easily removed by acidic foods and beverages, low pH mouthrinses, and some toothpaste detergents such as sodium lauryl sulfate or polyphosphates.
Measures to Combat Dentin Hypersensitivity
Understanding the mechanism described in the hydrodynamic theory provides two strategic approaches to manage the dentin hypersensitivity, including:
• reduce or stop the fluid movement in the tubules, or
• interfere with the neural transmission to the brain.
For the approach of occluding open dentin tubules and reducing fluid movement, the most commonly employed technologies include protein precipitants, calcium and phosphate precipitating agents, various crystallizing agents, bonding agents, and even surgical grafting of gingival tissue. Some of these technologies also lend themselves well to at-home products for application by the patient as well as those intended for professional application. Pastes and varnishes of high fluoride concentration (eg, a prescription toothpaste containing 5,000 ppm fluoride; a fluoride varnish containing 22,600 ppm fluoride) have been found to be effective in promoting mineral deposition and thus tubule occlusion leading to symptom relief. However, many products for in-office application are not supported by evidence derived from rigorously designed clinical trials. An innovative technology that mimics natural physiological properties of saliva to deposit mineral elements inside the open tubules has been introduced following such testing and publication of the results in peer-reviewed publications.9 The technology is based upon the amino acid arginine that occurs naturally in saliva and calcium carbonate. Together when formulated in a prophylaxis paste it has been shown to form a robust plug in dentin tubule orifices in laboratory studies and to provide significant relief of dentin hypersensitivity symptoms in clinical trials (Figure 5). One of the laboratory studies tested the resistance of the plug to dissolution by acids. Dentin was treated with the arginine-calcium carbonate desensitizing prophylaxis paste and then exposed to cola for a total of two minutes to stimulate consumption of an acidic beverage. The integrity of the dentin surface and the occluded tubules was examined by confocal laser scanning microscopy which showed the occluded tubules remain occluded after two minute exposure to cola, demonstrating the occluding layer is resistant to an acid challenge from a typical beverage product.10
The above materials can be applied at home by the patient or readily in the dental office and are thus simple and inexpensive but effective first lines of treatment. If on review of the case, the treatment has not been fully effective and the original diagnosis of dentin hypersensitivity is still supported, other procedures that are more invasive can be employed. These procedures include the application of a bonding agent, a filled or unfilled resin, or even a gingival graft. Clearly for widespread and generalized dentin hypersensitivity, a toothpaste or prophy paste provides ideal coverage whereas the more invasive procedures are typically limited by both access and cost to only a few isolated teeth.
For interfering with transmission of the neural impulse, the application of potassium nitrate is the most commonly used agent. Potassium ions have been shown to depolarize the nerve and prevent it from repolarizing and thus “firing.” Potassium nitrate reduces the excitability of the nerve and has an almost anesthetic effect. The scientific evidence supporting the mode of action of potassium salts is largely based on animal studies in which the intradental nerve activity could be reduced.11 Clinical studies with toothpastes containing 5% potassium nitrate have been shown to be effective in the relief of dentin hypersensitivity symptoms when applied by brushing twice daily.12 The effect has been shown to start slowly after 2 weeks and provide increasing relief after 8–12 weeks continued use.13 Care should be taken to instruct patients to use the paste twice a day and to stop the use of their regular paste, as it is the continued use of the potassium nitrate formula that enables a sufficient concentration of potassium ions to diffuse along the open tubule to reach the mechano-receptors and their A-delta nerve fibers in close proximity of the odontoblasts. Failure to control the symptoms is most likely to be a result of inadequate compliance. However if the patient’s sensitivity problem remains after using desensitizing toothpaste, the clinician should re-evaluate the differential diagnosis and consider in-office and more invasive types of treatment.
Conclusions
The symptoms of sensitive teeth are troublesome for most patients. However, not all patients bring those symptoms to the attention of their dental professional—for many reasons; instead they continue to suffer and manage the symptoms by various coping strategies.
Dentin hypersensitivity as a specific condition is becoming more prevalent in dental practice. The clinician is being challenged to provide quick relief to this discomfort.
Many remedies and products have been developed and brought into either in-office or at-home use. A number of these products have little or no evidence of clinical support for their manufacturer’s claims and some when used in isolation may take several weeks to bring about measurable relief.
Use of a clinically proven technology based upon the natural physiology of saliva and a calcium salt has been shown to offer immediate relief when applied like a prophylaxis paste. Between recall visits, this can be supported by use of a potassium nitrate–based toothpaste for twice daily use.
Finally, the clinician is advised to identify and fully address the underlying causes of hypersensitivity—exposed dentin as a result of either gingival recession or loss of enamel. Both conditions are a threat to the sustained longevity of the teeth and are often not diagnosed until they have resulted in a change in the normal and healthy appearance of the mouth. Dentin hypersensitivity should be regarded as a warning sign of either gingival recession or tooth surface loss. If these conditions are allowed to remain unchecked, the additional exposure of dentin can only be expected to result in further episodes of dentin hypersensitivity with all its potential negative impacts on a normal daily life.
References
1. Addy M. Dentine hypersensitivity: new perspectives on an old problem. Int Dent J. 2002;52(suppl 1):367-375.
2. Strassler HE, Drisko CL, Alexander DC. Dentin hypersensitivity: its inter-relationship to gingival recession and acid erosion. Compend Contin Educ Dent. 2008;29(spec issue):1-9.
3. Gandara BK, Truelove EL. Diagnosis and management of dental erosion. J Contemp Dent Recommendations Pract. 1999;1(1):16-23.
4. West NX. Detine Hypersensitivity. Monogr Oral Sci. 2006;20:173-189.
5. Holland GR, Narhi MN, Addy M, et al. Guidelines for the design and conduct of clinical trials on dentine hypersensitivity.
J Clin Periodontol. 1997;24:808-813.
6. Pashley DH, Tay FR, Haywood VB, Collins MA, Drisko CL. Dentin Hypersensitivity: Consensus-Based for the Diagnosis & Management of Dentin Hypersensitivity. Inside Dentistry (2008:4(9 spec iss):1-7.
7. Brännström M In: Anderson DJ, ed. Sensory Mechanisms in Dentine. Oxford; Pergamon Press; 1963.
8. Absi EG, Addy M, Adams D. Dentine hypersensitivity. A study of the patency of dentinal tubules in sensitive and non-sensitive cervical dentine. J Clin Perio. 1987;14(5):280-284.
9. Cummins D. Recent advances in dentin hypersensitivity: clinically proven treatments for instant and lasting sensitivity relief. Am J Dent. 2010;23(spec iss A):3A-13A.
10. Petrou I, Heu R, Stranick M, et al. A breakthrough therapy for dentin hypersensitivity: how dental products containing 8% arginine and calcium carbonate work to deliver effective relief of sensitive teeth. J Clin Dent. 2009;20(1):23-31.
11. Markowitz K, Bilotto G, Kim S. Decreasing intradental nerve activity in the cat with potassium and divalent cations. Arch Oral Biol. 1991;36(1):1-7.
12. Poulsen S, Errboe M, Lescay Mevil Y, Glenny AM. Potassium containing toothpastes for dentine hypersensitivity.
Cochrance Database Syst Rev. 2006;3:CD001476.
13. Nagata T, Ishida H, Shinohara H, et al. Clinical evaluation of a potassium nitrate dentifrice for the treatment of dentinal hypersensitivity. J Clin Periodontol. 1994;21(3):217-221.
Disclosure
The author received an honorarium from Colgate-Palmolive.