You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Dentin hypersensitivity is a sharp, acute pain that results from the exposure of dentin surfaces to stimuli, such as thermal, evaporative, tactile, osmotic, chemical, or electrical stimulus. It also cannot be associated with any other dental disease.1,2 A degree of dentin sensitivity is normal; however, hypersensitivity implies that the tooth is experiencing sensitivity that is greater than the usual sensitivity to various stimuli. Dentin hypersensitivity is a global oral health issue and a significant challenge for many dental professionals. Symptoms of dentin hypersensitivity are generally reported by the patient, difficult to describe, and challenging to accurately diagnose. Before making a diagnosis, other dental diseases must be ruled out first, such as dental caries, cracked-tooth syndrome, and defective restorations, among others.
Dentin hypersensitivity is a commonly presenting condition and can range from a minor inconvenience to the patient, to a near incapacitating quality-of-life disturbance. Zeola et al conducted a systematic review and meta-analysis and found that dentin hypersensitivity affects approximately 11.5% of people, and the average from all studies was 33.5% of people.3 The prevalence of hypersensitivity varies greatly in different studies, which can be partly explained by the differences in selection criteria and variety in diagnostic approaches or timeframes. The highest prevalence is seen in periodontal patients (approximately 60% to 98%), possibly due to the exposure of root surfaces and subsequent dentin tubule exposure as part of the periodontal disease process and treatment.4,5 Dentin hypersensitivity generally involves the facial surfaces near the cervical aspect of teeth and is most common in premolars and canines.6 A prudent practitioner must understand the etiology of dentin hypersensitivity and the underlying cause in each individual case in order to best treat a patient's sensitivity and/or pain.
Etiology of Dentin Hypersensitivity
Teeth are comprised of three main layers: the outer protective enamel layer; the supportive dentin layer, which also encompasses the roots; and, lastly, the internal pulp. Within the dentin layer are dentin tubules, which contain a lymph-like fluid and odontoblast processes. Dentin is composed of many microscopic tubular structures that extend outward from the pulp; these tubules are typically 0.5 µm to 2 µm in diameter. A plasma-like biological fluid is present in the dentin tubules, and movement of this fluid can trigger mechanoreceptors present on nerves located at the pulp, thereby eliciting a pain response.
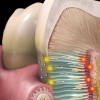
Many theories have been proposed to explain the mechanism involved in the etiology of dentin hypersensitivity. These include the transducer theory, modulation theory, "gate" control and vibration theory, and hydrodynamic theory. The latter, hydrodynamic theory, developed by Dr. Martin Brännström, is now widely accepted as the cause of tooth sensitivity.6 However, it must be noted that none of these mechanisms fully elucidate dentin hypersensitivity, indicating that other unexplained mechanisms possibly are responsible for causing the condition. The widely accepted hydrodynamic theory states that stimuli (thermal, chemical, tactile, or evaporative) are transmitted to the pulpal nerves by mechanical receptors due to movement of fluid within open dentin tubules.7 The fluid movement stimulates the small, myelinated A-delta fibers, which then transmit to the brain and result in the sensation of well-localized, sharp pain. A visual representation of the hydrodynamic theory is presented in Figure 1.
Based on the hydrodynamic theory, dentin hypersensitivity is a transient tooth pain. To exhibit a response to the stimuli, the tubules have to be open at both the dentin surface and the pulpal surface of the tooth. Anatomically, the areas of the tubules closer to the pulp chamber are wider and the number of tubules per unit area increases almost twofold from the outer surface to the pulp.8 Teeth affected by dentin hypersensitivity have a greater number of open tubules, almost eight times per unit area, compared with nonsensitive teeth.9
The most important factor affecting the fluid flow in dentin is the radius of the dentin tubules. If the radius is reduced by one-half, the fluid flow within the tubules falls to 1/16th of its original rate. Therefore, the creation of a smear layer or the occlusion of the tubules will significantly lessen sensitivity by reducing the radius of the open dentin tubules and causing a reduction in dentin tubule fluid flow.10
Generally, as a predisposing factor to dentin hypersensitivity, the dentin needs to become exposed, typically as a result of loss of enamel and/or gingival recession. The main cause of exposed tubules that lead to dentin hypersensitivity is gingival recession, which results in the exposure of root surfaces, loss of cementum and smear layer, and tooth wear.11 Gingival recession is often a sign of long-term traumatic brushing or chronic periodontitis.12 Another less common reason for gingival recession is acid erosion related to gastroesophogeal reflux disease, bulimia, or excessive consumption of acidic food and/or drinks. Dental bleaching, cracked teeth, and bruxism may also cause hypersensitivity.13,14
Diagnosis
The diagnosis of dentin hypersensitivity is challenging, because it is a diagnosis of exclusion; it is only reached after all other possible explanations for the patient's pain have been ruled out.1 Other conditions with symptoms of sensitivity include chipped teeth, cracked teeth, fractured restorations, dental caries, gingival inflammation, post-restorative sensitivity, marginal leakage, and pulpitis. Therefore, a thorough patient history and clinical examination are required to rule out these other conditions and reach a diagnosis of dentin hypersensitivity.
The clinician should look for exposed dentin to confirm the diagnosis when patients are complaining of hypersensitivity. Exposed dentin is most commonly seen in patients with periodontitis, leading to exposure of root surfaces. It can also be seen in patients with malocclusion (premature occlusal contacts), causing abfraction and/or attrition, and patients that brush aggressively causing abrasion of enamel. One study showed a significant association among non-carious cervical lesions (NCCLs), premature contacts, and consumption of wine and other alcoholic beverages; dentin hypersensitivity was associated with NCCLs, premature contacts, and the consumption of acidic fruits and juices.15
The reason(s) why tubules are exposed or open should be assessed during a visual examination of the teeth. Additionally, a detailed dietary history should be taken, as certain foods that are acidic may be causing erosion of enamel and exposure of tubules. Useful diagnostic tools and methods include a blast of air from the air/water syringe (thermal), a dental explorer (tactile), bite stress tests (eg, tooth sleuth), other thermal tests such as the use of refrigerant spray, and assessment of occlusion. These tests should be positive for pain provocation, but if the results are negative, no treatment for dentin hypersensitivity is indicated and another diagnosis should be explored. If an individual responds positively to only the bite stress test, a cracked tooth may be the underlying cause of the patient's hypersensitivity.
The dental pain experienced with dentin hypersensitivity is often sharp in character and short in duration. However, the response to stimuli varies from patient to patient. Factors such as individual pain tolerance, emotional state, and environment (eg, certain workplaces like a battery manufacturing facility, where employees may be exposed to sufuric acid mist that can be a cause of dental erosion and subsequent dentin sensitivity) can contribute to the variety of responses among patients.16 If the patient's history and examination is consistent with dentin hypersensitivity and the diagnosis has been confirmed, the patient may be treated accordingly. The steps a dental professional should take to diagnose a patient with dentin hypersensitivity are outlined in Figure 2.17
Management
There is no universally accepted "gold standard" treatment that reliably relieves the pain of dentin hypersensitivity in the long term,and, consequently, many treatment options for this condition have varying degrees of efficacy.18 If the diagnosis confirms dentin hypersensitivity in the absence of underlying diseases or structural problems of the tooth, the following steps may be initiated: (1) remove the risk factors by educating the patient about dietary acids and other oral care habits; (2) recommend different toothbrushing methods, remote from mealtime, if appropriate; subsequently, the practitioner should perform a follow-up to assess if the patient's dentin hypersensitivity persists. If the patient is still experiencing pain, then (3) initiate treatment by recommending a desensitizing agent for home use and/or applying topical desensitizing agents in-office. These noninvasive, simple treatments should be implemented before more invasive procedures are attempted.
At times, a more aggressive and invasive approach, such as mucogingival surgery, use of resins, or pulpectomy, may be necessary to either cover exposed tubules or devitalize the tooth. Noninvasive treatment is indicated for mild to moderate dentin hypersensitivity associated with several teeth, and invasive treatment may be appropriate in cases of severe dentin hypersensitivity associated with one or two teeth.19 In extreme cases, if the patient does not respond to the therapy and individual teeth are exhibiting the symptoms, endodontic therapy may be required.
An ideal desensitizing agent should provide rapid action with long-term effects; be non-irritating to the pulp, painless, and simple to apply; and not cause staining on the teeth.19 The two different purported mechanisms of action include occlusion of dentin tubules by use of a mechanical barrier or stimulation of peritubular or reactive dentin (eg, resins, varnishes, toothpastes) or stabilization of nerve fibers, which interferes with the transmission of nerve impulses.19-21 Examples of treatments for patients experiencing dentin hypersensitivity are listed in Table 1.
The use of sealers and restorations to reduce dentin hypersensitivity has been shown to be more effective in the short term versus long term. Brushing with desensitizing toothpaste is also effective but for long-term use of more than 6 months. A 2016 meta-analysis concluded that arginine-containing toothpastes are effective in the treatment of dentin hypersensitivity by promoting dentin tubule closure.22 Another meta-analysis examining desensitizing toothpastes found that there is sufficient evidence to support the use of toothpastes that contain potassium, stannous fluoride, potassium and stannous fluoride, calcium sodium phosphosilicate, or arginine for dentin hypersensitivity, but not the use of strontium-containing desensitizing toothpaste.23
Laser treatment is another option for patients experiencing dentin hypersensitivity. Laser is an acronym for "light amplification by stimulated emission of radiations." Various studies have shown that lasers can be used in the effective management of dentin hypersensitivity.24,25 The mechanism of action of lasers in treating dentin hypersensitivity is somewhat unclear. Some authors have shown that neodymium-doped yttrium aluminum garnet (Nd:YAG) and erbium-yttrium aluminum garnet (Er:YAG) laser application occluded dentin tubules leading to decreased hypersensitivity, lasting up to 6 months.25-27 Galium-aluminum-arsenide (GaAlA) laser is thought to act by affecting the neural transmission in the dentin tubules.28 It has also been proposed that lasers coagulate the proteins inside the dentin tubules and block the movement of fluid.25 Studies have reported that Nd:YAG, Er:YAG, and GaAlA laser therapy can reduce dentin hypersensitivity pain, but the evidence for their effectiveness is weak, as the reductions were not statistically different from those of a placebo.27,29 In addition to these equivocal results, lasers represent a more expensive and complex treatment modality.
Potential Treatments for Dentin Hypersensitivity
A self-applied, nontoxic paste that adheres to wet surfaces would be an ideal carrier for occluding agents that could encourage permanent closure of patent dentin tubules. One such polymer that fits these criteria is poly(dopamine methacrylamide-co-methoxyethyl acrylate) (poly[DMA-co-MEA]). It is a sticky gelatinous substance that is capable of adhering to moist surfaces and could act as an excellent carrier for a dentin tubule blocking agent. The filler for this carrier ideally would be small enough to fit into the open tubules and create a mineralized layer that would help bring about permanent relief of the pain caused by dentin hypersensitivity. Chen et al synthesized fluorhydroxyapatite crystals, which were recognized as being ideal as a filler for the poly(DMA-co-MEA) polymer, being of appropriate size and having the potential to release calcium, phosphate, and fluoride at acid pH.30 Further work on this novel, experimental desensitizing paste needs to be carried out, especially conductivity tests.
Another potential treatment modality is the use of dendrimers or artificial proteins. These proteins have large branches, which can be functionalized with molecules such as antimicrobial or anti-inflammatory agents. These agents would help to control the pulpal inflammation under sensitive dentin to provide immediate and, possibly, lasting pain relief. These dendrimers can be added to larger particles, which can be synthesized with calcium, phosphate, and fluoride and released as the particle degrades over time after entering the patent dentin tubule and gets exposed to various oral environmental conditions. This would help to calcify the patent tubules, forming a permanent barrier and potentially providing long-lasting relief.31
Conclusion
Dentin hypersensitivity is a prevalent problem that affects many dental patients. When patients present with symptoms of this condition, they should be examined and informed of the treatment options available to relieve them of sensitivity and/or pain. Because their daily habits may be contributing to the problem, patients may play a role in the process of dentin hypersensitivity and should be informed of the possible need to change certain behaviors, otherwise the condition may persist. A thorough history and clinical examination will provide the practitioner the information needed to diagnose and treat the patient.
In most cases the initial cause of dentin hypersensitivity is gingival recession with the exposure of dentin tubules. Once the tubules are exposed the patient is susceptible to pain in response to thermal, tactile, or osmotic stimuli. Desensitizing treatments should be delivered systematically.
Prevention and over-the-counter treatments, including the use of desensitizing toothpastes, should be implemented before more invasive treatments are initiated, and these prevention measures may later be supplemented with in-office treatments, if necessary. With comprehensive understanding of the etiology of dentin hypersensitivity, along with effective preventive and treatment options, the dental healthcare team can provide excellent care to patients with this irritating and often painful condition. Dental professionals must be knowledgeable about oral signs and symptoms of dentin hypersensitivity in order to diagnose the problem and educate and treat patients experiencing symptoms.
About the Authors
Justin Felix
Fourth year dental student at the Faculty of Dentistry, University of Toronto, Toronto, Ontario, Canada
Aviv Ouanounou, BSc, MSc, DDS
Assistant Professor, Department of Clinical Sciences (Pharmacology and Preventive Dentistry), Faculty of Dentistry, University of Toronto, Toronto, Ontario, Canada
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Türp JC. Discussion: how can we improve diagnosis of dentin hypersensitivity in the dental office? Clin Oral Investig. 2013;17(suppl 1):S53-S54.
2. Canadian Advisory Board on Dentin Hypersensitivity. Consensus-based recommendations for the diagnosis and management of dentin hypersensitivity. J Can Dent Assoc. 2003;69(4):221-226.
3. Favaro Zeola L, Soares PV, Cunha-Cruz J. Prevalence of dentin hypersensitivity: systematic review and meta-analysis. J Dent. 2019;81:1-6. doi: 10.1016/j.jdent.2018.12.015.
4. Chabanski MB, Gillan DG, Bulman JS, Newman HN. Clinical evaluation of cervical dentine sensitivity in a population of patients referred to a specialist periodontology department: a pilot study. J Oral Rehabil. 1997;24(9):666-672.
5. von Troil, B, Needleman I, Sanz M. A systematic review of the prevalence of root sensitivity following periodontal therapy. J Clin Periodontol. 2002;29(suppl 3):173-177.
6. Addy M. Etiology and clinical implications of dentine hypersensitivity. Dent Clin North Am. 1990;34(3):503-514.
7. Nishida M, Murayama Y, Nomura Y, et al. Hypersensitivity of the exposed root surface after surgical periodontal treatment. Japanese Journal of Periodontology. 1976;18(4):502-510.
8. Berman LH. Dentinal sensation and hypersensitivity. A review of mechanisms and treatment alternatives. J Periodontol. 1985;56(4):216-222.
9. Absi EG, Addy M, Adams D. Dentine hypersensitivity. A study of the patency of dentinal tubules in sensitive and non-sensitive cervical dentine. J Clin Periodontol. 1987;14(5):280-284.
10. Michelich V, Pashley DH, Whitford GM. Dentin permeability: a comparison of functional versus anatomical tubular radii. J Dent Res. 1978;57(11-12):1019-1024.
11. Petersson LG. The role of fluoride in the preventive management of dentin hypersensitivity and root caries. Clin Oral Investig. 2013;17(suppl 1):S63-S71.
12. Hargreaves KM, Cohen SR. Cohen's Pathways of the Pulp. 10th ed. St. Louis, MO: Mosby Elsevier; 2010.
13. Hattab FN, Yassin OM. Etiology and diagnosis of tooth wear: a literature review and presentation of selected cases. Int J Prosthodont. 2000;13(2):101-107.
14. Nathanson D. Vital tooth bleaching: sensitivity and pulpal considerations. J Am Dent Assoc.1997;128(suppl):41S-44S.
15. Yoshizaki KT, Francisconi-Dos-Rios LF, Sobral MA, et al. Clinical features and factors associated with non-carious cervical lesions and dentin hypersensitivity. J Oral Rehabil. 2017;44(2):112-118.
16. Dugmore CR, Rock WP. A multifactorial analysis of factors associated with dental erosion. Br Dent J. 2004;196(5):283-286.
17. Limeback H, ed. Comprehensive Preventive Dentistry. Ames, IA: Wiley-Blackwell; 2012.
18. Schmidlin PR, Sahrmann P. Current management of dentin hypersensitivity. Clin Oral Investig. 2013;17(suppl 1):S55-S59.
19. Karim BF, Gillam DG. The efficacy of strontium and potassium toothpastes in treating dentine hypersensitivity: a systematic review. Int J Dent. 2013;2013:573258. doi: 10.1155/2013/573258.
20. Bal J, Kundalgurki S. Tooth sensitivity prevention and treatment. Oral Health. 1999;89(2):33-41.
21. Miglani S, Aggarwal V, Ahuja B. Dentin hypersensitivity: recent trends in management. J Conserv Dent. 2010;13(4):218-224.
22. Yang ZY, Wang F, Lu K, et al. Arginine-containing desensitizing toothpaste for the treatment of dentin hypersensitivity: a meta-analysis. Clin Cosmet Investig Dent. 2016;8:1-14.
23. Bae JH, Kim YK, Myung SK. Desensitizing toothpaste versus placebo for dentin hypersensitivity: a systematic review and meta-analysis. J Clin Periodontol. 2015;42(2):131-141.
24. Kimura Y, Wilder-Smith P, Yonaga K, Matsumoto K. Treatment of dentine hypersensitivity by lasers: a review. J Clin Periodontol. 2000;27(10):715-721.
25. McCarthy D, Gillam DG, Pearson GJ. In vitro effects of laser radiation on dentine surfaces. J Dent Res. 1997;76:1756-1756.
26. Schwarz F, Arweiler N, Georg T, Reich E. Desensitizing effects of an Er: YAG laser on hypersensitive dentine. J Clin Periodontol. 2002;29(3):211-215.
27. Birang R, Poursamimi J, Gutknecht N, et al. Comparative evaluation of the effects of Nd:YAG and Er:YAG laser in dentin hypersensitivity treatment. Lasers Med Sci. 2007;22(1):21-24.
28. Corona SA, Nascimento TN, Catirse AB, et al. Clinical evaluation of low-level laser therapy and fluoride varnish for treating cervical dentinal hypersensitivity. J Oral Rehabil. 2003;30(12):1183-1189.
29. Sgolastra F, Petrucci A, Gatto R, Monaco A. Effectiveness of laser in dentinal hypersensitivity treatment: a systematic review. J Endod. 2011;37(3):297-303.
30. Chen H, Tang Z, Liu J, et al. Acellular synthesis of a human enamel-like microstructure. Advanced Materials. 2006;18(14):1846-1851.
31. Chang S, Chen H, Liu J, et al. Synthesis of a potentially bioactive, hydroxyapatite-nucleating molecule. Calcif Tissue Int. 2006;78(1):55-61.