You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Performing clinical dentistry involves static posture, precise and repetitive motions, long work hours, and sub-optimal ergonomics.1,2 Among dental hygienists and dentists the prevalence of musculoskeletal disorders (MSDs) ranges from 64% to 93%, with repetitive movements and prolonged static postures listed as major risk factors.3-5 A study in the United Kingdom highlighted the risk to the careers of dental professionals as the authors reported that the most frequent reason for premature retirement among dentists was MSDs.6 According to the World Health Organization, work-related MSDs are "disorders or injuries affecting muscles, tendons, joints, ligaments and bones mainly caused by mechanical overload of the respective biological structures. Potential overload of tissues results from high intensity forces or torques acting on and inside the body."7
The types of MSDs commonly encountered by clinicians involve: neck and shoulder disorders, hand and wrist disorders, and back disorders.2 Focusing on hand and wrist disorders, dental hygienists and dentists suffer from more hand, wrist, and arm pain than the general population.8-10 Within the hand and wrist disorders, carpal tunnel syndrome (also called median nerve compression) is the most common MSD and is often the result of a combination of factors that may increase pressure on the median nerve and tendons in the carpal tunnel, rather than a problem with the nerve itself.10 Symptoms can produce discomfort in the hand and forearm and usually include numbness, tingling, or pain in the thumb, index, middle, and half of the ring finger, but not the little finger. Carpal tunnel syndrome may be the result of several causes, including: past history of trauma to the wrist, an overactive pituitary gland, an underactive thyroid gland, and rheumatoid arthritis.11 Other health-related risk factors involved in the development of carpal tunnel syndrome include: gender (females are three times as likely to develop carpal tunnel syndrome), diabetes, and obesity.10 Work-related risk factors for carpal tunnel syndrome include: mechanical stress to the hand and wrist, forceful exertion, repetitive motions, and prolonged static postures defined as maintaining the same position or posture throughout an exertion.7 For the dental clinician, activities such as flexing of the wrist forward, forceful gripping of small instruments, repetitive motions for long periods of time, and vibration have been implicated in the development of carpal tunnel syndrome symptoms.8,10
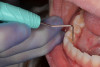
A study by Rice found that 71% of dentists experienced symptoms, although only 7% were diagnosed with carpal tunnel syndrome.12 This finding was also reported by Hamann and colleagues, where the prevalence of carpal tunnel syndrome symptoms was higher among dentists than in the general population.8 Another study by the American Dental Association found that 1 in 10 dentists had been diagnosed with a repetitive motion disorder, causing 19% to require surgery and 40% to work reduced hours.13 Proposed strategies for reducing carpal tunnel syndrome symptoms in dental clinicians include: using fitted gloves, larger handled instruments, pacing of work activity including breaks to prevent extended wrist flexion, improved wrist posture to reduce stress on the median nerve, and a night-time wrist splint.8Additional strategies suggested by another author include: adequate finger rests, using textured grips to reduce pinch strength, using sharp hand instruments to decrease work force, reducing cord pullback or tubing torque, and frequent stretch breaks11(Figure 1 and Figure 2). Currently, the ADA has a webpage devoted to "Reducing Hand Pain" that lists examples of motions that may aggravate hand pain and tips for lessening the demands of the hand as well as a recomvmendation to see a physician for medical evaluation and treatment if pain continues to worsen.14
Hygienists Are More at Risk Compared to Dentists
All members of the clinical dental team are at risk for development of MSDs, however dental hygienists are disproportionally affected compared to dentists.9 Studies by Rucker and colleagues found that 86% of dental hygienists compared to 67% of dentists reported MSD pain within the previous year.15,16The Rucker studies also reported that 75% of dental hygienists reported hand pain specifically compared to 38% of dentists. Several other studies have reported the prevalence of carpal tunnel syndrome in dental hygienists; with rates of 6.4% to 11%; 23%; and 50% being reported.17-20 Specific risk factors for dental hygienists proposed in a review article by Johnson and Kanji were listed as: awkward and static postures, repetitive movements, poor ergonomics, pinch-grasp, forceful exertions, vibration, and insufficient breaks.21
A possible means to decrease pinch force and reduce procedure time includes the use of ultrasonic instruments.22 However, the vibration of ultrasonic instruments may still be a risk factor of MSD and development of carpal tunnel syndrome.10,17,21,23 In many cases, hygiene treatment procedures involve both manual (i.e., hand instruments) and ultrasonic instruments, and whenever possible a combination of both techniques should be used to help vary hand positioning, reduce muscle workload, and provide intermittent rest to hand muscles specifically those involved with pinch force.10
Why Do We Polish Teeth During the Prophylaxis Visit?
Since the late 1970s, the notion that every tooth during every routine prophylaxis should be polished has been replaced by the "selective polishing theory" that asserts that polishing should only be performed on teeth with extrinsic stain.24,25 In addition, while research has shown that loss of enamel is minimal following coronal polishing, improper coronal polishing can cause significant damage to gingival tissues, exposed dentin and cementum, enamel, and especially restorations.26,27 Despite the theory of "selective polishing," full-mouth polishing is routinely performed as a component of a dental prophylaxis, most likely because of patient expectations. As a result, the term "selective polishing" has been updated to "essential selective polishing" to reinforce that if dental hygienists are routinely coronal polishing teeth, they should select the most appropriate polishing or cleaning agents according to the patient's individual needs.28,29
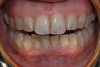
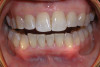
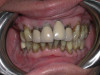
Dental hygienists and dentists should seek to reserve the coronal polishing procedure for the clinical situations that warrant it (removal of extrinsic stain, plaque, and biofilm). When coronal polishing is indicated, the use of appropriate prophylaxis paste grit or cleaning agent is advisable. Clinicians should also be aware of situations where coronal polishing may be contraindicated, such as: the absence of extrinsic stains, patients with acute periodontal infections, on esthetic restorations, for patients with severe tooth sensitivity, amelogenesis imperfecta, enamel demineralization, enamel hypocalcification, enamel hypoplasia, and exposed cementum24,28 (Figure 3 and Figure 4).
In addition to using both manual and ultrasonic instrumentation to help vary hand position and reduce muscle workload during the prophylaxis procedure, if clinicians are more selective when delivering coronal polishing then vibration can also be minimized over the workday. Further, by utilizing technology that can also help to prevent cord pullback and drag, pinch force, and muscle fatigue associated with the traditional prophylaxis handpieces, hygienists and dentists can further reduce risk factors for MSD symptoms.30
Air polishing is another option for removal of extrinsic stain and is an important part of the hygiene armamentarium. Compared to polishing with a rubber cup, the advantages of using air polishing include more efficient stain removal, in less time, with diminished dentin hypersensitivity, and less operator fatigue.31,32 The contraindications to air polishing can include: certain medical conditions (e.g., restricted sodium diets, respiratory, renal or metabolic disease), use on root surfaces, use on composites or porcelains, and use around ceramic or metal orthodontic brackets24,31,33,34 (Figure 5 and Figure 6). Advances in the latest powders used in air polishing may diminish some of these contraindications in the future (e.g., the use of glycine, the use of reduced air pressure).
A significant hazard to air polishing is the increased risk of aerosols. The use of rotary handpieces (both high- and low-speed), air abrasion, lasers, and ultrasonic units create a cloud of particles and fluid that may contain infectious materials from the treatment site and dental unit water lines. Exposure of dental personnel to this potentially infectious airborne material via aerosol and splatter has long been a concern in dentistry. The authors of a 2004 article in the Journal of the American Dental Association stated, "While, as with all infection control procedures, it is impossible to completely eliminate the risk posed by dental aerosols, it is possible to minimize the risk with relatively simple and inexpensive precautions."35
Aerosol is defined as small particles less than 50 microns in diameter that can stay airborne for an extended period of time before settling onto a surface. Splatter consists of larger particles (>50 microns in diameter) that are forcibly ejected from the working area and quickly fall onto a surface or floor because they are too large to remain airborne. Recommended procedures to minimize aerosol and splatter generation during dental procedures include universal barrier precautions, a pre-procedure rinse or pre-procedure toothbrushing, a rubber dam where possible, and use of high vacuum evacuation (HVE) suction.34,35,36
An Innovation in Prophy Handpieces
Prophy handpieces have historically been air-driven via tubing and may be heavy and unergonomic (e.g., slow-speed motor combined with a torque multiplier and straight nose cone). Even dedicated prophy handpieces (e.g., Nupro RDH™ [Dentsply Sirona], Ultrapro® Tx Air [Ultradent]) may still cause cord drag despite lighter weight and improved ergonomics. Cord drag or "cord catching" occurs when the weight and resistance of the dental tubing increases stress and muscle workload during instrumentation.30
A study by McCombs and Russell compared the muscle loads required during simulated tooth polishing using a corded versus a cordless handpiece.30 Electromyography (EMG) was used to measure the activity of four muscles involved in high pinch force. The results showed a reduced EMG for three out of the four muscles tested when the cordless handpiece was used, but the intensity of muscle workload between the corded and cordless handpieces was not statistically different. The biggest difference was an average 30-second reduction in polishing time with the cordless handpiece, which over the course of a workday would reduce duration of muscle workload, an important factor in preventing MSDs. The dental hygienists most preferred the cordless handpiece over the corded handpieces used in the study and when queried listed a lack of cord, weight and balance, and low noise as the main reasons for the preference.
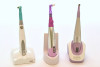
In 2011, Dentsply Sirona introduced the first cordless prophy handpiece, originally named the Midwest® RDH Freedom® Cordless Prophy System (Dentsply Professional) and more recently renamed the Nupro Freedom Cordless Prophy System. The original system included a motor component, metal sheath, charging base, and Bluetooth foot pedal, whereas the newer version can be used with or without a foot pedal.37Both use proprietary disposable prophy angles. In 2015, DentalEZ introduced the iStar™ Cordless Prophylaxis Handpiece, which is compatible with any prophy angle. The iStar is push-button operated and has variable speeds from 500 rpm to 2,500 rpm, but it is non-sterilizable with infection prevention mediated by disposable sleeves. Nupro, on the other hand, has variable speeds up to 3,000 rpm and uses sterilizable sheaths and disposable barriers for infection prevention (Figure 7 and Figure 8).
In 2019, Premier Dental introduced the AeroPro® Cordless Prophy Handpiece System (Figure 7 and Figure 8). It is compatible with any disposable prophy angle and allows the angle to be easily rotated 360° for improved intraoral access. As per the manufacturer, AeroPro is "ergonomic and lightweight with a well-balanced design, featuring a textured grip for reduced pinch strength and hand fatigue"38 (Figure 9 and Figure 10). It is controlled using a single button, features ChargeSMART™ technology for rapid charging and all-day battery life, and infection prevention is via autoclavable sheaths and disposable barriers. It has three speeds: 500 rpm, 1,500 rpm, and 2,500 rpm.
An article by Guignon in 2021 compared the six prophy handpeices currently on the market: Young™ Infinity, Permier AeroPro®, DentalEZ™ iStar, Dentsply Sirona Nupro Freedom, NSK iProphy Mobile, and Pac-Dent™ Promate CL.39 Despite all six handpieces being designed to use a rotating disposable prophy cup, they varied by design, dimensions, weight, foot pedal versus fingertip button control, rpm, charging, and infection control protocol. The author writes, "Some feel cordless polishers are not powerful enough. Simply pressing down harder creates more hand strain without enhancing stain removal. The goal of polishing is not to remove industrial strength stains that have been around for years. It is easier to break up heavy stain with a power scaler and remove remaining bits and pieces with a polisher." The speeds of the six polishers ranged from 500 rpm on low speed to a maximum of 2,500 rpm to 4,000 rpm depending on the unit, and the weight ranged from 90 grams to 121 grams.
Conclusions
Because of the nature of clinical dentistry-precise and repetitive motions, static posture, sub-optimal ergonomics, and long work hours-all members of the clinical team are at risk for development of MSDs. Dental hygienists may be at an increased risk for MSDs compared to dentists and must practice preventive strategies to maintain hand and musculoskeletal health. Appreciating that an effective dental hygiene program is an integral component of a successful dental practice and comprehensive patient care, hygienists should seek clinical equipment that can help reduce muscle workload and duration. Cordless prophy handpieces offer a meaningful innovation over corded predecessors and should be considered a worthwhile upgrade for the safe and ergonomic delivery of hygiene care.
About the Author
Jason H. Goodchild, DMD
Associate Clinical Professor
Department of Oral and Maxillofacial Surgery
Creighton University School of Dentistry
Omaha, Nebraska
Adjunct Assistant Professor
Department of Diagnostic Sciences
Rutgers School of Dental Medicine
Newark, New Jersey
Private Practice
Jenkintown, Pennsylvania
References
1. Zaerian M. Musculoskeletal disorders and the impacts on the dental professional. OralHealth website. February 1, 2019. https://www.oralhealthgroup.com/features/musculoskeletal-disorders-and-the-impacts-on-the-dental-professional/. Accessed November 11, 2022.
2. Chopra A. Musculoskeletal disorders in dentistry - a review. JSM Dent.2014;2(3):1032-1035.
3. Hayes MJ, Cockrell D, Smith DR. A systematic review of musculoskeletal disorders among dental professionals. Int J Dent Hyg. 2009;7(3):159-165.
4. Padhye NM, Padhye AM, Gupta HS. Effect of pre-procedural chair-side finger stretches on pinch strength amongst dental cohort - a biomechanical study. J Clin Diagn Res.2017;11(4):ZC82-ZC85.
5. McCombs GB, Russell DM. Reducing muscle workload. Dimensions of Dental Hygiene.2016;14(04):24-26, 29. https://dimensionsofdentalhygiene.com/article/reducing-muscle-workload/. Accessed November 11, 2022.
6. Burke FJ, Main JR, Freeman R. The practice of dentistry: an assessment of reasons for premature retirement. Br Dent J.1997;182(7):250-254.
7. World Health Organization. Preventing musculoskeletal disorders in the workplace. Protecting Workers' Health Series No. 5. June 23, 2003. https://www.who.int/publications/i/item/preventing-musculoskeletal-disorders-in-the-workplace. Accessed November 11, 2022.
8. Hamann C, Werner RA, Franzblau A, Rogers PA, Siew C, Gruninger S. Prevalence of carpal tunnel syndrome and median mononeuropathy among dentists. J Am Dent Assoc. 2001;132(2):163-170.
9. Hayes MJ, Smith DR, Cockrell D. An international review of musculoskeletal disorders in the dental hygiene profession. Int Dent J. 2010;60(5):343-352.
10. Carpal Tunnel Syndrome Fact Sheet. National Institute of Neurological Disorders and Stroke website. https://www.ninds.nih.gov/carpal-tunnel-syndrome-fact-sheet. Updated July 25, 2022. Accessed October 18, 2022.
11. Valachi B. Getting the upper hand on pain: preventing hand and wrist pain syndromes on dental professionals. PennWell. 2010. Available at: https://www.pdffiller.com/6633291-fillable-getting-the-upper-hand-on-pain-preventing-hand-and-wrist-pain-syndromes-in-dental-professionals-form. Accessed November 16, 2022.
12. Rice VJ, Nindel B, Pentikis JS. Dental workers, musculoskeletal cumulative trauma, and carpal tunnel syndrome: who is at risk? A pilot study. Int J Occup Saf Ergon. 1996;2(3):218-233.
13. American Dental Association Survey Center. 1997 Survey of Current Issues in Dentistry: Repetitive Motion Injuries. Chicago, IL: American Dental Association; 1997:2-8.
14. Reducing hand pain. ADA website. https://success.ada.org/en/wellness/reducing-hand-pain. Accessed November 14, 2022.
15. Rucker L. Evaluation of the Preventive Impact of Surgical Ergonomics Training and Surgical magnification. Vancouver, BC: Workers' Compensation Board of British Columbia. 2001. https://www.worksafebc.com/en/resources/about-us/research/finding-solutions-archive/evaluation-of-the-preventive-impact-of-surgical-ergonomics-training-magnification?lang=en. Accessed November 14. 2022.
16. Rucker LM, Sunell S. Ergonomic risk factors associated with clinical dentistry. J Calif Dent Assoc.2002;30(2):139-146.
17. Sanders MA, Turcotte CM. Strategies to reduce work-related musculoskeletal disorders in dental hygienists: two case studies. J Hand Ther. 2002;15(4):363-374.
18. Morse TF, Michalak-Turcotte C, Atwood-Sanders M, et al. A pilot study of hand and arm musculoskeletal disorders in dental hygiene students. J Dent Hyg. 2003;77(3):173-179.
19. Anton D, Rosecrance J, Merlino L, Cook T. Prevalence of musculoskeletal symptoms and carpal tunnel syndrome among dental hygienists. Am J Ind Med.2002;42(3):248-257.
20. Lalumandier JA, McPhee SD, Riddle S, Shulman JD, Daigle WW. Carpal tunnel syndrome effect on Army dental personnel. Mil Med.2000;165(3):372-378.
21. Johnson CR, Kanji Z. The impact of occupation-related musculoskeletal disorders on dental hygienists. Can J Dent Hyg. 2016;50(2):72-79.
22.Dong H, Barr A, Loomer P, Rempel D. The effects of finger rest positions on hand muscle load and pinch force in simulated dental hygiene work. J Dent Educ.2005;69(4):453-460.
23. Akesson I, Lundborg G, Horstmann V, Skerfving S. Neuropathy in female dental personnel exposed to high frequency vibrations. Occup Environ Med. 1995;52(2):116-123.
24. Sawai MA, Bhardwaj A, Jafri Z, Sultan N, Daing A. Tooth polishing: the current status. J Indian Soc Periodontol. 2015;19(4):375-380.
25. Barnes CM. The science of polishing. Dimensions of Dental Hygiene. 2009;7(11):18-20, 22. Available at: https://dimensionsofdentalhygiene.com/article/the-science-of-polishing/. Accessed November 14, 2022.
26. Pence SD, Chambers DA, van Tets IG, Wolf RC, Pfeiffer DC. Repetitive coronal polishing yields minimal enamel loss. J Dent Hyg.2011;85(4):348-357.
27. Christensen GJ. Prophy pastes: helpful and harmful. Clinicians Report. 2018;11(6):1-8.
28. Barnes C. Shining a new light on selective polishing. Dimensions in Dental Hygiene. 2012;10(3):42, 44.
29. Boyd LD, Mallonee LF, Wyche CJ. Wilkins' Clinical Practice of the Dental Hygienist. 13th Edition. Burlington, MA: Jones & Bartlett Learning; 2021. p 729-744.
30. McCombs G, Russell DM. Comparison of corded and cordless handpieces on forearm muscle activity, procedure time and ease of use during simulated tooth polishing. J Dent Hyg.2014;88(6):386-393.
31. Graumann SJ, Sensat ML, Stoltenberg JL. Air polishing: a review of current literature. J Dent Hyg. 2013;87(4):173-180.
32. Barnes CM. Air polishing: a mainstay for dental
hygiene. PennWell. 2013. Available at: https://www.yumpu.com/en/document/view/22671110/air-polishing-a-mainstay-for-dental-hygiene-ineedcecom. Accessed November 14, 2022.
33. Johnson K. Air polishing has changed - so why hasn't the dental hygiene curriculum? Dentistry IQ. August 16, 2016. https://www.dentistryiq.com/articles/2016/08/air-polishing-has-changed-so-why-hasn-t-the-dental-hygiene-curriculum.html. Accessed November 14, 2022.
34. Gutmann ME. Air polishing: a comprehensive review of the literature. J Dent Hyg.1998;72(3):47-56.
35. Harrel SK, Molinari J. Aerosols and splatter in dentistry. J Am Dent Assoc. 2004;135(4):429-437.
36. Bentley CD, Burkhart NW, Crawford JJ. Evaluating spatter and aerosol contamination during dental procedures. J Am Dent Assoc.1994;125(5):579-584.
37. Dryer M. Coronal polishing: the evolution of handpieces offers a new spin on dental hygiene services. RDH. June 1, 2017. https://www.rdhmag.com/articles/print/volume-37/issue-6/contents/coronal-polishing.html. Accessed November 14, 2022.
38. AeroPro® Cordless Handpiece. Premier Dental Products website. https://www.premierdentalco.com/product/hygienepreventative/cordless-handpieces/aeropro-systems/aeropro-cordless-handpiece-system/. Accessed November 14, 2022.
39. Guignon AN. Cordless polishers: another tool in the toolbox. RDH. September 30, 2021. https://www.rdhmag.com/ergonomics/article/14209844/cordless-polishers-another-tool-in-the-toolbox. Accessed November 14, 2022.