You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Diet is defined as the habitual eating patterns of an individual, whereas nutrition refers to the science of food intake and biological processes.1,2 Nutrients can be categorized into macronutrients (proteins, carbohydrates, fats), micronutrients (minerals, vitamins), and water.1 Examples of macronutrients are illustrated in Figure 1.
Inflammation is the body's protective response to a challenge, such as infection and trauma. While acute inflammation results in an immune response that leads to resolution with removal of the stimuli, chronic inflammation is central to the underlying pathophysiology of many chronic diseases.3 Furthermore, chronic systemic inflammation alters the use and consumption of various macronutrients (ie, fats, proteins, carbohydrates) by promoting the breakdown of protein and fat while stimulating the liver to produce more acute phase response proteins (APP).3 It is well-established that increased caloric intake or poor quality of diet with nutrient deficiencies is related to systemic conditions such as diabetes and obesity.4
In the adult population, one of the most common chronic inflammatory conditions is periodontal diseases. Many studies have shown that significant periodontal disease is associated with a significant increase in serum levels of inflammatory mediators and pro-inflammatory cytokines.3 This demonstrates the link between periodontal diseases, inflammation, and macronutrient intake.4 Therefore, dental healthcare providers (DHCP) have an important role in advocating healthful diets to improve both oral and systemic health.
When diet and dental health are considered together, the predominant thought is usually about caries and sugar. It is well established that the intake of carbohydrates is subsequently metabolized by oral microorganisms. Acidic end products are released and come into contact with tooth structures, namely enamel and dentin, causing their demineralization. Upon continual exposure to this acidic insult, caries develops.2
However, diet and nutrition also impact periodontal health, and the maintenance of periodontal health relies on a diet that provides sufficient macronutrients and micronutrients.2 This article focuses specifically on macronutrients and their association with periodontal health and disease.
Periodontal Diseases: Influences of Macronutrient Consumption
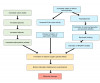
The pathogenesis of periodontal disease is complex and multifactorial. Although plaque biofilm is necessary for the onset of periodontitis, the tissue destruction mostly results from the abnormal host immuno-inflammatory response.5 As in many chronic inflammatory conditions, a state of hyperinflammation is apparent.5 One important factor in periodontal disease progression is oxidative stress, due to an overproduction of reactive oxygen species (ROS) that overwhelms the antioxidant defenses in the body (Figure 2).1,5 This imbalance causes problems for normal redox signaling and can result in molecular damage, and this process may be influenced by the types and amounts of macronutrients consumed.1
An overall caloric excess can cause excess glucose production.5 Through a series of metabolic pathways, including insulin metabolism and lipoprotein synthesis in the liver, caloric excess results in increases in free fatty acids and a decrease in lipolysis, which, over a sustained period of time, can result in increased adiposity.5 As adipose tissue increases, this activates transcription factors that upregulate the production of pro-inflammatory cytokines.1 Specifically, adipose tissue secretes adipocytokines, including tumor necrosis factor, interleukin-1, and interleukin-6, which can induce the production of ROS.5 An association between postprandial oxidative stress and increased levels of C-reactive protein (a marker of systemic inflammation) has also been shown to be associated with increased adiposity.5
Furthermore, intake of macronutrients may contribute to oxidative stress and inflammation.1 This is referred to as postprandial oxidative stress or "meal-induced inflammation."5 For example, a diet that includes an increased amount of refined carbohydrates will result in an excess amount of superoxide radicals, which are byproducts of ATP synthesis in the Krebs cycle.1 The superoxide radicals can be components for generation of ROS further downstream.5 In addition, increased consumption of refined carbohydrates can lead to hyperglycemia and result in the formation of advanced glycation end products (AGEs).1,5 AGEs bind to their receptors (RAGE) and are responsible for a range of changes in the host, including neutrophil defects, hyperinflammatory responsive monocytes, and increased release of pro-inflammatory cytokines.1 Increased intake of saturated fats will result in the formation of low-density lipoprotein cholesterol, which, when oxidized, will bind to toll-like receptor 4 on neutrophils.1,5 The neutrophil binding activates NADPH-oxidase, which will increase the production of ROS.1
An increased incidence of periodontal disease progression has also been shown in individuals who have a high intake of omega-6 fats.6 Studies have also demonstrated increased gingival bleeding in individuals who have high intakes of sugars and carbohydrates when compared with individuals who followed a "Stone Age" diet low in refined carbohydrates (even in patients who ceased oral home care measures such as toothbrushing and flossing).7-9 The type of fat consumed may be important in its influence on periodontal health. For instance, while omega-6 fats have been implicated in the progression of periodontal disease, omega-3 fats have been shown to have the opposite effect.1,5 Omega-3 fats lower postprandial triglyceride levels, inhibit lipid mediators of inflammation (eg, prostaglandin E2 and cyclo-oxygenase), downregulate the pro-inflammatory gene expression, increase antioxidant activity, and produce pro-resolving lipid mediators (eg, resolvins and protectins).1,5
Periodontal lesions and tooth loss are frequent symptoms of Kwashiorkor, which is a condition caused by severe lack of protein intake.10 Additionally, an observational study found a lower incidence of significant periodontitis in individuals who had a high intake of casein and whey proteins (commonly found in dairy products).9
Current Eating Patterns of Americans
The US Department of Health and Human Services and the US Department of Agriculture periodically update and publish guidelines for diet and nutrition for Americans.11 These guidelines make recommendations for a diet to meet nutritional goals while remaining below caloric limits in order to help individuals achieve a healthy lifestyle and reduce the risk of the onset of chronic diseases.11 The most recent guidelines (2015-2020) highlight the current eating pattern of Americans.11 In general, most American do not meet the recommendations for vegetables, fruits, dairy, and oils, while they have a disproportionate consumption of added sugars, saturated fats, and sodium, resulting in excessive caloric intake.11 It is clear that the typical American diet is not in alignment with the guidelines and that the recommended nutritional goals are not being met.
In brief, dietary recommendations made by the US Department of Health and Human Services and the US Department of Agriculture for 2015-2020 include11:
• Increase total vegetable intake from all vegetable subgroups: dark-green vegetables, red and orange vegetables, legumes, starchy vegetables, other vegetables,
• Increase fruit intake (mostly whole fruits, in nutrient-dense forms),
• Shift to make half of total grains consumed to be whole grains: switch refined for whole-grain versions,
• Increase dairy intake in fat-free or low-fat forms,
• Increase the variety of proteins (switch meats/poultry/eggs to more seafood and more nuts, seeds, and soy products),
• Shift from solid fats to oils,
• Limit the amount of sugars, saturated fats, and sodium.
Nutritional Counseling in the Dental Practice
Diet is a modifiable risk factor. As dental professionals are able to screen for oral disease, such as dental caries and periodontal diseases, they can assess the contribution of diet to such diseases. Tools such as the Rapid Eating Assessment for Participants (shortened version) can be used chairside to assess a patient's nutritional intake.12 In addition, because of the two-way associations between periodontal diseases and systemic diseases, educating patients and advocating diets that are more compatible with periodontal health is a necessary aspect of oral healthcare. Based on the evidence provided above, a diet that can facilitate periodontal health is low in refined carbohydrates, but is high in whole grains, omega-3 fats, casein and whey proteins, and in foods with antioxidant properties. Because of the multifactorial nature of periodontal diseases, it is important to emphasize that modification of nutrient intake alone will not be able to prevent or arrest progression of periodontal diseases.2
When comparing the recommendations made in this article from a periodontal perspective with the 2015-2020 Dietary Guidelines for Americans, many similarities are noted, particularly regarding the decreased intake of refined carbohydrates (and subsequent increased intake of whole grain carbohydrates), increased dairy intake (casein and whey proteins), and reduced sugar intake. However, one notable difference is the recommendations about vegetable oils. The 2015-2020 Dietary Guidelines for Americans recommend vegetable oils instead of solid fats from the standpoint of cardiovascular disease and excess caloric intake.11 However, studies on vegetable oils (omega-6 fats) have demonstrated that omega-6 fats promote inflammation and can increase the incidence of progression of periodontal disease.6,8 Therefore, the benefits and the risks of omega-6 fats should be weighed prior to modification of diet in this aspect. For patients who have a cardiovascular disease diagnosis, suitable substitutes can be suggested for vegetable oils with lower omega-6 content.
Periodontitis is characterized by microbially associated, host-mediated inflammation resulting in loss of periodontal tissues. Plaque biofilm is required for the onset of periodontitis, but the resulting tissue destruction is primarily due to abnormal host immune response to inflammation.5 One important factor that contributes to the state of hyperinflammation is oxidative stress, a result of ROS overpowering the body's antioxidant defenses.1,5 An individual's intake of macronutrients can contribute to oxidative stress and inflammatory response by either up-regulating or down-regulating it.1 These relationships necessitate consideration of the adjunctive role of diet in periodontitis.3 Evidence suggests a diet not only low in refined carbohydrates but also one that includes whole-grain carbohydrates and is high in omega-3 fats, casein and whey proteins, and foods with antioxidant properties can downregulate the destructive inflammatory response of the host and facilitate periodontal health.1,5,9,13 Today, still little is known about the role of nutrition in periodontitis. With rapid advances in molecular biology and nutritional genomics, there is an opportunity for better understanding the interface between nutrition and periodontal disease in the future.3
References
1. Raindi D. Nutrition and periodontal disease. Dent Update. 2016;43(1):66-68, 71-62.
2. Hujoel PP, Lingström P. Nutrition, dental caries and periodontal disease: a narrative review. J Clin Periodontol. 2017;44(Suppl 18):S79-S84.
3. Enwonwu CO, Ritchie CS. Nutrition and inflammatory markers. J Am Dent Assoc. 2007;138(1):70-73.
4. Hamasaki T, Kitamura M, Kawashita Y, et al. Periodontal disease and percentage of calories from fat using national data. J Periodontal Res. 2017;521):114-121.
5. Chapple ILC. Potential mechanisms underpinning the nutritional modulation of periodontal inflammation. J Am Dent Assoc. 2009;140(2):178-184.
6. Iwasaki M, Taylor GW, Moynihan P, et al. Dietary ratio of n-6 to n-3 polyunsaturated fatty acids and periodontal disease in community-based older Japanese: a 3-year follow-up study. Prostaglandins Leukot Essent Fatty Acids. 2011;85(2):107-112.
7. Hujoel P. Dietary carbohydrates and dental-systemic diseases. J Dent Res. 2009;88(6):490-502.
8. Woelber JP, Bremer K, Vach K, et al. An oral health optimized diet can reduce gingival and periodontal inflammation in humans - a randomized controlled pilot study. BMC Oral Health. 2016;17(1):28.
9. Adegboye AR, Boucher BJ, Kongstad J, Fiehn NE, Christensen LB, Heitmann BL. Calcium, vitamin D, casein and whey protein intakes and periodontitis among Danish adults. Public Health Nutr. 2016;19(3):503-510.
10. Seck T, Moreau JL. Dental lesions. After-effects of Kwashiorkor [in French]. Inf Dent. 1982;64(13):1259-1268.
11. U.S. Department of Health and Human Services and U.S. Department of Agriculture. 2015 - 2020 Dietary Guidelines for Americans. 8th Edition. December 2015. https://health.gov/our-work/food-and-nutrition/2015-2020-dietary-guidelines/. Accessed August 13, 2020.
12. Segal-Isaacson CJ, Wylie-Rosett J, Gans KM. Validation of a short dietary assessment questionnaire: the Rapid Eating and Activity Assessment for Participants short version (REAP-S). Diabetes Educ. 2004;30(5):774-778.
13. Baumgartner S, Imfeld T, Schicht O, et al. The impact of the stone age diet on gingival conditions in the absence of oral hygiene. J Periodontol. 2009;80(5):759-768.