You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Since their introduction into the dental armamentarium in 1965 by Dr. PI Brånemark, endosseous dental implants have seen a significant increase in their prevalence as tooth replacement options. The American Academy of Implant Dentistry states that roughly 3 million individuals receive 5 million dental implants annually.1 Given the high numbers of implants placed and dental practitioners involved in implant dentistry, it will become ever more commonplace to encounter patients who have received implant therapy.2 An advantage of this increase in implant placement is expanded learning about what allows for successful implant therapy and incremental improvements to implant fixtures, prostheses, and protocols that can allow patients to achieve better function and implant health. These improvements include improved digital image capture, novel surgical technologies, and advanced implant fixture and restorative materials. These advances have improved dental implant longevity and management of surgical and prosthetic complications. In addition to these technological advances, practitioners also continue to refine their assessment methods for dental implant therapy. As such, it is critical that dental practitioners involved in dental implant therapy understand conditions that may reduce implant success and the methods that may mitigate such risks. Dental healthcare providers seek to deliver thorough treatment planning that addresses patient concerns and is focused on the patient as a whole. In order to provide individualized patient care, it is critical to be aware of patient- and site-specific risks, including systemic conditions, oral health status, and previous implant failure history. An understanding of the multidisciplinary care required for long-term success and the critical importance of ongoing implant maintenance will allow the dental team to improve the quality of treatment, making the overall patient experience more positive.
Success vs Survival
While implant survival, defined as an implant present and in function regardless of attachment loss, is a critical component of patient satisfaction with implant therapies, it does not assess ongoing inflammatory conditions, prosthetic stability, and/or esthetic concerns regarding implant therapies.3,4 As patients become more savvy about dental implants, their expectations for esthetic, phonetic, and functional success continue to increase. While many criteria, including Albrektsson, have been used to identify success rates for dental implants, new standards continue to evolve.3 More recently, the 2017 American Academy of Periodontology (AAP)/European Federation of Periodontology (EFP) World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions (WWDC 2017) defined criteria for peri-implant health, peri-implant mucositis, and peri-implantitis.5 Peri-implant health has been characterized as the absence of inflammation and bone loss around the implant site.5,6 This includes no signs of erythema, bleeding upon gentle probing, nor swelling and suppuration.5,6 While it is not possible to determine peri-implant health from probing depth measurements alone, due to implant anatomy and dimensions of peri-implant mucosa, it is still necessary to record probing depths and attachment levels to monitor long term health, as increasing probing depth over time has been associated with peri-implant diseases.7,8 Peri-implant mucositis is characterized by the clinical signs of inflammation absent in health.5,9 Bleeding upon gentle probing is necessary to constitute peri-implant mucositis, while erythema, swelling, and suppuration may also be present.5,9 In peri-implant mucositis, increased probing depth can be seen due to mucosal swelling and a decreased resistance by connective tissue prior to onset of bone loss.5,9 These inflammatory signs are initiated by plaque accumulation in the peri-implant tissues, but the histologic lesion that develops, the inflammatory markers present, and the time to resolution of clinical and histologic inflammation were greater at sites with experimental peri-implant mucositis than those with experimental gingivitis.10 Peri-implantitis has been characterized as a plaque-induced pathological condition with inflammatory signs in the mucosa and progressive loss of supporting bone structure.5,11 Inflammatory signs noted are similar to those of peri-implant mucositis, including bleeding and/or suppuration upon gentle probing, erythema, and swelling.5,11 The presence of bone loss beyond the crestal bone level changes of initial remodeling results in increased probing depths over time and radiographic bone loss..5,11 Figure 1 illustrates the details of similarities and differences in each classification.
Given the increased prevalence of dental implants in the US population, it is important for oral healthcare providers to assess prosthesis stability, radiographic bone loss, and absence of infection in the peri-implant soft tissues regularly. Furthermore, it is also critical to assess phonetic and esthetic success and overall patient satisfaction with dental implants and prostheses. An investigation by Papaspyridakos and colleagues focused on prosthetic level success and patient satisfaction, providing dental practitioners with a broader view of how dental implant therapy can improve.12 Prosthetic success and patient satisfaction are closely related when considering esthetic implants.12 While dental implant fixtures serve as synthetic tooth roots to support the dental implant prostheses, they must also align with the remaining dentition and/or oral tissues. Peri-implant tissue health, keratinization, tissue position-including height and volume, color, and contour-should all be evaluated in relation to surrounding and contralateral tissues to ensure optimal esthetics. Restorations themselves can be assessed in terms of color, form, texture, size, and optical properties. The recognition of multifactorial aspects of implant success and their impact on long-term satisfaction can inform interdisciplinary approaches to solutions for individual patients.
Although the main goal for any dental procedure is to achieve success, treatments often fall short of this ultimate goal. In understanding the causes of such failures, clinicians are able to predict outcomes and potentially improve patient satisfaction if these are taken into account during the treatment planning phase. Early failures (before osteointegration) and late failures (after osteointegration) appear to be caused by different factors.5 Furthermore, complications can also be classified as biologic or prosthetic and have differing etiologies, but can result in similar levels of dissatisfaction for patients and practitioners. The most common cause of implant failure is attributed to peri-implantitis,13 and primary peri-implantitis prevention is critical to establishing the highest levels of success.
Biologic Complications
Peri-implant mucositis and peri-implantitis are the two main peri-implant diseases experienced by patients, with an average prevalence of 46.83% and 19.83% respectively.12-14 These diseases have been shown to be directly related to microbial invasion and plaque accumulation. Peri-implant mucositis is characterized by bleeding and/or suppuration on gentle probing independent of an increased probing depth compared to previous examinations and the absence of bone loss beyond crestal bone level changes resulting from initial bone remodeling.9,14,15 Peri-implant mucositis is often considered analogous to gingivitis, but experimental biofilm accumulation results in a more pronounced inflammatory response in peri-implant mucosa versus that seen in gingival tissues, and this inflammatory lesion is also more persistent and difficult to reverse when biofilm is removed.10,15 Risk indicators for the development of peri-implant mucositis include patient-delivered oral hygiene levels, compliance with maintenance protocols, implant prosthetic design, dimensions of peri-implant keratinized tissues, and retained cement.9 Peri-implantitis can be defined as the presence of bleeding or suppuration upon gentle probing, increase in probing depth upon periodic evaluations, and the presence of bone loss beyond the crestal level after initial remodeling.11 Risk factors for peri-implantitis include a history of periodontitis, smoking, diabetes mellitus/glycemic control, poor plaque control, and/or a lack of regular maintenance therapy.16 These risk factors and indicators are outlined in Table 1 (online at aegisdentalnetwork.com/go/idh521), highlighting the level of impact that they may have on developing or worsening peri-implantitis. The common etiologic factors for both inflammatory implant conditions are periopathogenic bacteria, and a focus on controlling existing periodontal disease and eliminating reservoirs for such bacteria prior to implant therapy is a critical component to long-term success.5,9,11 Furthermore, the interdisciplinary dental team can work together to design cleansable prostheses and to ensure ongoing maintenance care for patients who have dental implants.
Prosthetic Complications
Prosthetic and occlusal complications do not have underlying microbiological etiology and do not, in most cases, jeopardize the osseointegration of the dental implant. They are nevertheless a clinical problem during the practice of treating implant patients. A recent review identified six categories of technical or mechanical failures: loosening of screws, screw fracture, fracture of framework, fracture of abutment, chipping/fracture of veneering material, and decementation.17 While prosthetic complications, as reported in this retrospective analysis, were not as frequent as biologic complications, the impact on patients was still substantial. The overall incidence of technical or mechanical complications for all implants in partially edentulous patients was 10.8% for single implant restorations (ISCs) and 16.1% for fixed partial implant-supported prostheses (FPID) over approximately a 5-year period.17 Furthermore, the most commonly seen prosthetic complications for ISCs and FPIDs were screw loosening and veneering material fracture, respectively.17 These complications can result in significant time and expense to repair and can, if left untreated, lead to prosthesis mobility, plaque accumulation, and potentially to biologic complications as well.
It should also be noted that prosthetic design can influence cleansability and pre-dispose dental implants to poor oral hygiene and/or inflammatory implant diseases. Excess cement remnants have been shown to increase the risk for developing peri-implantitis.16 Excess cement has the potential to create microbial adherence that could initiate the immune response, leading to inflammation and tissue destruction.18,19 Additional complications include inadequate connections between implants and prostheses, loose screws due to inadequate torque strength, overcontouring of certain restorations, early or excessive loading, and restoration fractures. Complications that are specific to the prostheses may be more easily managed than those that include the implant itself, but all these complications impact patient perception of implants and their success.
Treatment Planning
Planning for dental implant therapy begins with a comprehensive evaluation of the patient's medical and dental history and an assessment of overall risk. Many factors can increase the risks for peri-implantitis and implant failure when not recognized and/or treated adequately. Additionally, identifying the patient's desires and expectations after implant placement allow practitioners to manage expectations and assess risks for functional and esthetic compromise. Dental hygienists play a crucial role in patient selection and risk assessment associated with dental implant treatment plans. The intimate understanding of patients' overall systemic health and compliance with oral hygiene and maintenance recommendations should be part of the overall implant planning team. A patient-centered approach that weighs the individualized risks of treatment and customizes the outcomes to meet those risks is critical to overall implant success.
In clinical practice, successful dental implant therapy allows practitioners to help patients achieve optimal oral health and esthetic outcomes, which rely heavily upon many patient, site, and treatment-related factors. Factors related to patients' systemic health, patient behaviors, site-specific anatomy, restoration type, and fixture type have all been indicated in the development of peri-implant diseases and worsening treatment outcomes after therapy.5 Proper patient selection and pre-procedural planning to reduce or eliminate these risk factors may reduce the overall need for peri-implant disease treatment.
In addition to a thorough assessment of systemic medical conditions, a comprehensive dental examination can establish periodontal health status and conditions, as well as local anatomical factors that may impact the dental implant treatment plan. Periodontally compromised patients are noted to be at highest risk for developing peri-implantitis.5,11,16,20 Conclusions made at the WWDC 2017 show that pathologic conditions in the oral environment, such as the persistence of chronic periodontal disease and poor plaque control, could induce changes in the ecosystem that may favor the colonization of pathogenic microorganisms at implant sites.5 Prior to implant placement, patients should have established periodontal health and stability and acceptable oral hygiene/plaque control to reduce the risk of contamination of implants with bacterial etiology. While controlled periodontal disease reduces the risk, patients with a history of periodontitis remain at a higher risk for development of peri-implantitis.5 Given this increased risk, such patients may require shorter maintenance intervals, in-depth oral hygiene instructions, alterations of prosthetic design to allow easier delivery of oral hygiene, and demonstrated long-term plaque control before initiating implant therapy. Dental hygienists and the care they deliver to such patients is requisite to long-term success. With successful management of peri-implantitis risk factors, an increase in dental implant success rates should be achieved.
Esthetic success is also important in meeting patient expectations and achieving high levels of satisfaction. Both local and systemic factors can negatively impact esthetic success. Table 2 (online at aegisdentalnetwork.com/go/idh521) illustrates the main areas of esthetic concern and how they influence overall risk as outlined by the International Team for Implantology's "Esthetic Risk Assessment."21 Complete assessment of local factors and patient expectations is critical to overall patient-assessed success. Intraoral and extraoral photography and videography can help capture lip positioning and mobility, while intraoral impressions can allow for assessment of site-specific dimensions and periodontal phenotype. A deep understanding of the patient's expectations, however, requires thorough conversations and may include the use of digital image manipulation to demonstrate a realistic outcome.
The Role of Diagnostic Tools in Treatment Planning
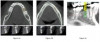
Advances in dental technology have allowed enhanced precision in dental implant treatment planning. Radiographic imaging is necessary to diagnose dental, periodontal, and implant health, but there are some restrictions with standard two-dimensional images. Traditional radiographs serve a great purpose in monitoring bone height over longer periods of time, leading to an understanding of the progression of bone remodeling and loss. While this information is diagnostic with supplemental clinical information, two-dimensional images cannot capture all dimensions of bone volume that are critical when planning dental implant surgery. The introduction of cone beam computerized tomography (CBCT) imaging to dental implant therapy has revolutionized how dental practitioners are able to plan all aspects of treatment from diagnosis through surgical procedures to prosthetic outcomes and evaluations. The use of CBCT for implant treatment planning allows for advanced assessment of the three-dimensional hard and soft tissue volumes and the potential for digital implant placement.22-24 This technology can allow for improved surgical and prosthetic precision, diagnoses, and outcomes (Figure 2).22-24
Pairing bone-level data from CBCT and gingival/mucosal contours from digital scanning impressions can allow for a comprehensive model to be used in treatment planning.23-25 Information gathered from CBCT along with digital scanning systems can also be used to fabricate custom surgical guides, abutments, and temporary and/or final prostheses. The possibilities with this technology are exciting, and the ability to plan each step of therapy can allow for precise assessment along with management of many variables that have the potential to lead to implant failure and/or peri-implant diseases. Additionally, digital smile design software utilizes this information to create a realistic esthetic result demonstrating expected outcomes to patients and to allow for implant placement with a restorative end goal in mind.25 This technology can allow patients to better understand the treatment process and visualize their final smile, which can manage patient expectations and lead to improved treatment success. Utilizing technology and combining it with the underlying biologic understanding of implant and patient-related factors is associated with implant success. This type of comprehensive approach to dental implant treatment planning has the potential to improve outcomes for patients and providers.
Summary
Identification of patient and site-level risks for dental implant therapy is a fundamental step in the long-term success of dental implants and patient satisfaction. While these initial evaluations may appear cumbersome, they allow the dental team to best identify patients who are good candidates for implant therapy and give dental healthcare providers the opportunity to establish oral health and wellness prior to progressing to dental implant therapy.
Taking a patient-centered, comprehensive approach allows dental team members to anticipate treatment outcomes and intercede to improve success rates. An interdisciplinary approach allows the dental team as a whole to understand each aspect of treatment in order to achieve overall success. The treatment planning process may be regarded as the most important step in dental implant therapy, so that patients and the dental team have an understanding of the risks and rewards.
About the Authors
Steven Sheibley
D4 Student Dentist,
University of Alabama at Birmingham School of Dentistry
Birmingham, AL
Maria L. Geisinger, DDS, MS
Professor and Director
Advanced Education Program in Periodontology,
University of Alabama at Birmingham School of Dentistry
Birmingham, AL
References
1. Tooth Implant vs Bridge: What Top Dentists Are Recommending. ADA Marketplace. https://marketplace.ada.org/blog/tooth-implant-vs-bridge-what-top-dentists-are-recommending/. Accessed February 26, 2021.
2. Elani HW, Starr JR, Da Silva JD, Gallucci GO. Trends in dental implant use in the U.S., 1999-2016, and projections to 2026. J Dent Res. 2018;97(13):1424-1430.
3. Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):11-25.
4. Smith DE, Zarb GA. Criteria for success of osseointegrated endosseous implants. J Prosthet Dent1989;62(5):567-572.
5. Berglundh T, Armitage G, Araujo MG, et al. Peri‐implant diseases and conditions: Consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri‐Implant Diseases and Conditions. J Periodontol. 2018;89(Suppl 1):S313- S318.
6. Araujo MG, Lindhe J. Peri-implant health. J Periodontol.2018;89(Suppl 1):S249-256.
7. Schwarz F, Becker K, Sahm N, et al. The prevalence of peri-implant disease for two-piece implants with an internal tube-in-tube connection: A cross-sectional analysis of 512 implants. Clin Oral Implants Res.2017;28(1):24-28.
8. Berglundh T, Zitzmann NU, Donati M. Are peri-implantitis lesions different from periodontitis lesions? J Clin Periodontol2011;38(Suppl 11):188-202.
9. Heitz-Mayfield LJA, Salvi GE. Peri-implant mucositis. J Periodontol.2018;89(Suppl 1):S257-S266.
10. Zitzmann NU, Berglundh T, Marinello CP, Lindhe J. Experimental peri-implant mucositis in man. J Clin Periodontol.2001;28(6):517-523.
11. Schwarz F, Derks J, Monje A, Wang H‐L. Peri‐implantitis. J Periodontol. 2018;89(Suppl 1):S267-S290.
12. Papaspyridakos P, Chen CJ, Singh M, et al. Success criteria in implant dentistry: A systematic review. J Dent Res. 2012;91(3):242-248.
13. Koldsland OC, Scheie AA, Aass AM. Prevalence of peri-implantitis related to severity of the disease with different degrees of bone loss. J Periodontol.2010;81(2):231-238.
14. Lee CT, Huang YW, Zhu L, Weltman R. Prevalences of peri-implantitis and peri-implant mucositis: systematic review and meta-analysis. J Dent. 2017;62:1-12.
15. Pontoriero R, Tonelli MP, Carnevale G, et al. Experimentally induced peri-implant mucositis. A clinical study in humans. Clin Oral Implants Res.1994;5(4):254-259.
16. Renvert S, Quirynen M. Risk indicators for peri-implantitis. A narrative review. Clin Oral Implants Res. 2015;26(Suppl 11):15-44.
17. Sadid-Zadeh R, Kutkut A, Kim H. Prosthetic failure in implant dentistry. Dent Clin North Am.2015;59(1):195-214.
18. Staubli N, Walter C, Schmidt JC, et al. Excess cement and the risk of peri-implant disease - a systematic review. Clin Oral Implants Res. 2017;28(10):1278-1290.
19. Wilson TG Jr. The positive relationship between excess cement and peri-implant disease: A prospective clinical endoscopic study. J Periodontol.2009;80(9):1388-1392.
20. Daubert DM, Weinstein BF, Bordin S, et al. Prevalence and predictive factors for peri-implant disease and implant failure: a cross-sectional analysis. J Periodontal. 2015;86(3):337-347.
21. Martin W, Morton C, Buser D. Pre-operative analysis and prosthetic treatment planning in esthetic implant dentistry. In: Buser D, Belser U, Wismeijer D, eds. ITI Treatment Guide. Vol 1: Implant Therapy in the Esthetic Zone for Single Tooth Replacements. New Malden, Surrey, UK: Quintessence Publishing Co Ltd; 2007:9-24.
22. Jacobs R, Vranckx M, Vanderstuyft T, Quirynen M, Salmon B. CBCT vs other imaging modalities to assess peri-implant bone and diagnose complications: a systematic review. Eur J Oral Implantol. 2018;11(Suppl 1):77-92.
23. Jacobs R, Salmon B, Codari M, Hassan B, Bornstein MM. Cone beam computed tomography in implant dentistry: recommendations for clinical use. BMC Oral Health. 2018;18(1):88.
24. Haiderali Z. The role of CBCT in implant dentistry: uses, benefits, and limitations. Br Dent J.2020;228:560-561.
25. Cervino G, Fiorillo L, Arzukanyan AV, et al. Dental restorative digital workflow: digital smile design from aesthetic to function. Dent J.2019;7(2):30.
26. ITI's SAC Classification in Implant Dentistry. Chen S, Dawson A, eds. Esthetic Modifiers. In: The SAC Classification in Implant Dentistry. Berlin: Quintessence Publishing Co., Ltd; 2009:15.